Lymphedema is a long-term condition that results from the obstruction or damage of lymphatic vessels or lymph nodes. This obstruction or damage causes lymph fluid to build up in affected parts of the body. Swelling, skin changes and other chronic health problems can progress if the condition goes untreated. Common causes of lymphedema include cancer, cancer treatment or trauma that reduce the effectiveness of lymphatic drainage. A physician is responsible for diagnosing lymphedema and creating a management program for the patient to control the swelling and discomfort common for this condition. Dr. Sacks and Dr. Anolik are members of the Division of Plastic and Reconstructive Surgery at Washington University School of Medicine, in which lymphedema treatment is one of ten clinical programs.
On this page:
Lymphedema Symptoms, Causes and Prevention: Frequently Asked Questions
What is lymphedema?
Lymphedema is a condition that causes swelling in certain parts of the body, such as the arms or legs, due to a build-up of lymph fluid that collects in the soft tissue. As part of the lymphatic system, lymph fluid keeps the body healthy by collecting pathogens and waste, and carrying these harmful substances to be filtered by the immune system before they are removed from the body. The lymphatic system is composed of lymph fluid, lymphatic vessels (pipes for carrying the fluid), and lymph nodes (like a port for the fluid, where it is filtered). If the lymphatic vessels are not properly carrying lymph fluid through the body or a lymph node is unable to drain lymph fluid, this results in unregulated fluid build-up. The build-up causes the characteristic soft tissue swelling of lymphedema.
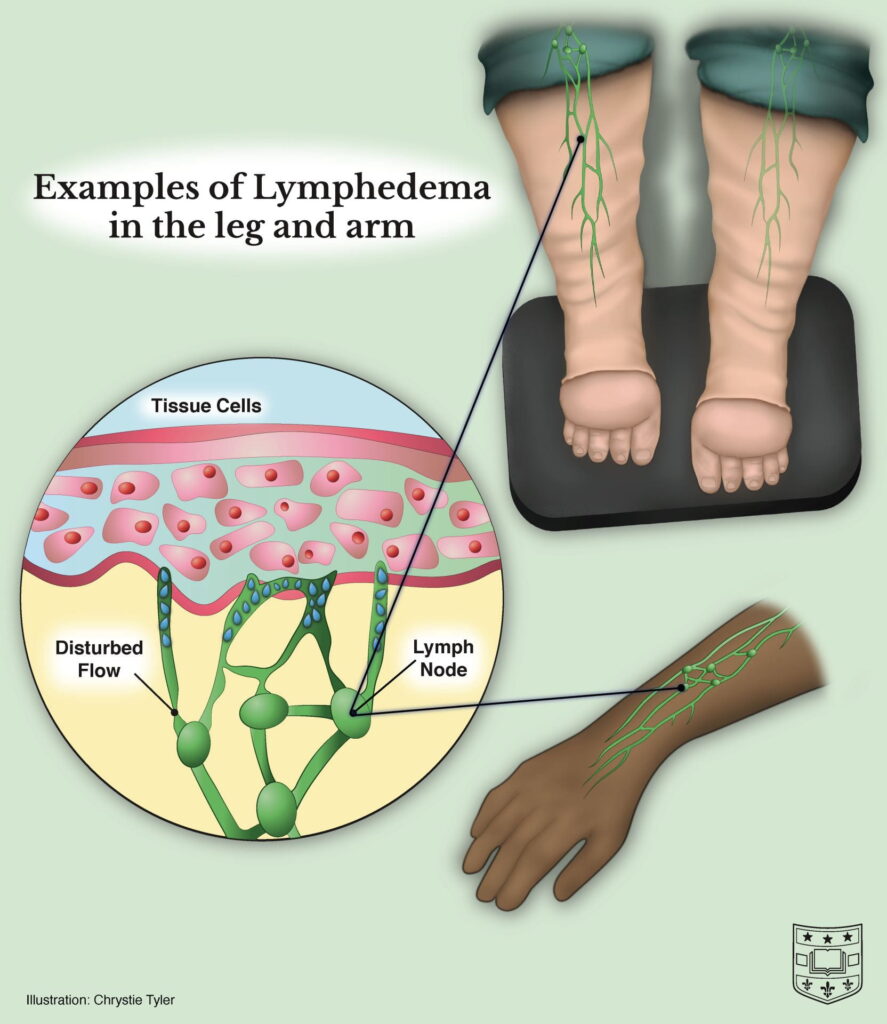
What are the symptoms of lymphedema? What are its stages?
General symptoms of lymphedema include:
- The progressive swelling of an arm, leg or other part of your body
- A sensation of heaviness, aching or discomfort in the affected limb
- Restricted movement or range of motion
- Clothing or jewelry feeling tighter or no longer fitting where swelling has occurred
- Skin feeling tight and tingling, burning or itching
- Skin appearing thicker or leathery (known as fibrosis)
- Recurring infections in the same area of the body
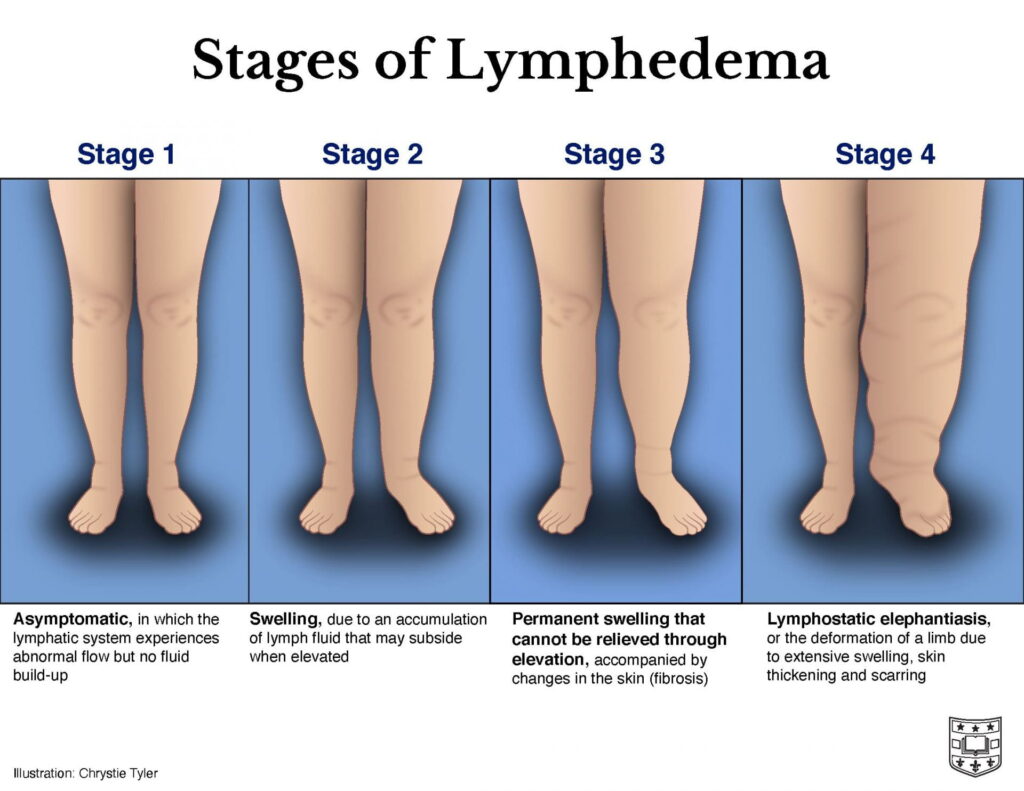
Stages of lymphedema follow its trajectory of swelling and skin damage. Four general stages are recognized in the progress of lymphedema:
- Stage 1: Asymptomatic, in which the lymphatic system experiences abnormal flow but no fluid build-up.
- Stage 2: Swelling, due to an accumulation of lymph fluid that may subside when elevated.
- Stage 3: Permanent swelling that cannot be relieved through elevation, accompanied by changes in the skin (fibrosis).
- Stage 4: Lymphostatic elephantiasis, or the deformation of a limb due to extensive swelling, skin thickening and scarring.
Can lymphedema be painful? Does it cause other problems?
Lymphedema can be a painful condition due to the persistence and increased severity of swelling. The reduction of swelling is necessary to reduce discomfort.
Having lymphedema can also increase the chance for developing other illnesses, such as infection. Because active immune cells can not reach the part of the body affected by lymphedema, infection can proliferate. Wounds may also heal more slowly in this area, and the joints of these regions can feel sore or stiff.
Another complication of lymphedema is lymphangiosarcoma, which is a rare form of cancer in the soft tissue. This cancer occurs when long-term, severe lymphedema is left untreated. Signs of lymphangiosarcoma include bruise-like color changes to the skin of the swollen body part.
What causes lymphedema? How does lymphedema start?
Lymphedema comes in primary or secondary forms. In primary lymphedema, the condition occurs on its own due to a problem with proper operation of the lymphatic system. Secondary lymphedema is caused by another disease or condition. This form of lymphedema is more common.
Primary lymphedema is a congenital (inherited genetic) condition caused by issues with the development of the lymphatic system. Specific conditions that cause primary lymphedema are Milroy’s disease (congenital lymphedema), Meige’s disease (lymphedema praecox), and late-onset lymphedema (lymphedema tarda).
The most common causes of secondary lymphedema are cancer and cancer treatment. The removal of a lymph node or lymphatic vessels as part of cancer treatment can cause lymph fluid to build up in the surrounding area. Radiation can also damage lymphatic vessels. A cancerous tumor may also block the lymphatic system before it is removed and result in lymphedema.
Breast cancer is often associated with upper-body and arm lymphedema due to the removal of axillary (underarm) lymph nodes. Other cancers in the uterus, ovaries or prostate may result in lower-limb lymphedema. Lymphoma, cancer in the immune system, can also cause lymphedema. High-dose radiation therapy and surgery for cancer in the neck or head is likely to promote lymphedema in these areas.
Secondary lymphedema may result from infection of the lymph nodes or vessels, causing damage and limiting functionality. This is more common in tropical or subtropical regions of the world. Other trauma to the lymphatic system, such as crushing injuries or burns, can disrupt drainage when lymphatic vessels or nodes are damaged. Scar tissue can create a barrier that prevents proper drainage.
The swelling of lymphedema can develop quickly or progress over several months. Mild lymphedema might go unnoticed, and lymphedema caused by cancer treatment may not occur until months or years later. Patients should consult with a doctor if they notice any bodily swelling that has become persistent or noticeably progressed.

Are there risk factors for having lymphedema?
Beyond the primary and secondary causes listed above, there are risk factors for developing lymphedema. These include older age, excess weight (obesity) and arthritis (rheumatoid or psoriatic). Other cardiac or vascular impairments, such as congestive heart failure or insufficient circulation, can also impair circulation of lymph fluid and cause lymphedema. Finally, kidney disease decreases the ability of the kidney to remove extra fluid and waste products, causing a back-up of lymph fluid.
Can you prevent lymphedema? If so, how?
Primary lymphedema can not be prevented, as it occurs due to inherited conditions of the lymphatic system. Symptoms can be minimized if treated early.
Secondary lymphedema may be prevented, depending on its cause. Lymphedema caused by surgery or radiation can be reduced with the help of a doctor, who will consider how medical procedures are performed to lessen the potential for lymphedema. After these procedures, methods of reducing lymphedema include exercise, compression and massage therapy. Washington University surgeons, oncologists and other specialists work together to prevent or manage secondary lymphedema after cancer.
If you have lymphedema, how can you prevent further health problems?
Lymphedema management is necessary to prevent infections and encourage circulation in the affected body region. To prevent infections, skin must be kept clean and moisturized, and any cuts or scrapes should be cleaned, covered with antibacterial medicine and bandaged. To promote lymph fluid movement, patients should not wear tight clothing or jewelry on the affected limb, and it is advised to elevate it above the heart when possible. Gravity will aid in the drainage of lymph fluid from a raised limb. More advanced treatment and therapy for lymphedema should be taken under the direction of a doctor or surgeon who specializes in treating this condition.
Washington University Lymphedema Experts
The team of Washington University surgeons, including Dr. Sacks and Dr. Anolik have built an advanced program for treating lymphedema and providing management services. Surgeons with the Division of Plastic and Reconstructive Surgery provide expert surgical care for patients with lymphedema. They collaborate with radiology, medicine, and occupational and physical therapy teams. Lymphedema surgeons and therapists see patients at the Center for Advanced Medicine and Barnes-Jewish West County Hospital.
For more information about lymphedema treatment or to make an appointment with Dr. Sacks or Dr. Anolik at the Center for Advanced Medicine or Barnes-Jewish West County Hospital, please call 314-362-7388.
Learn more about the Division of Plastic and Reconstructive Surgery at plasticsurgery.wustl.edu.
