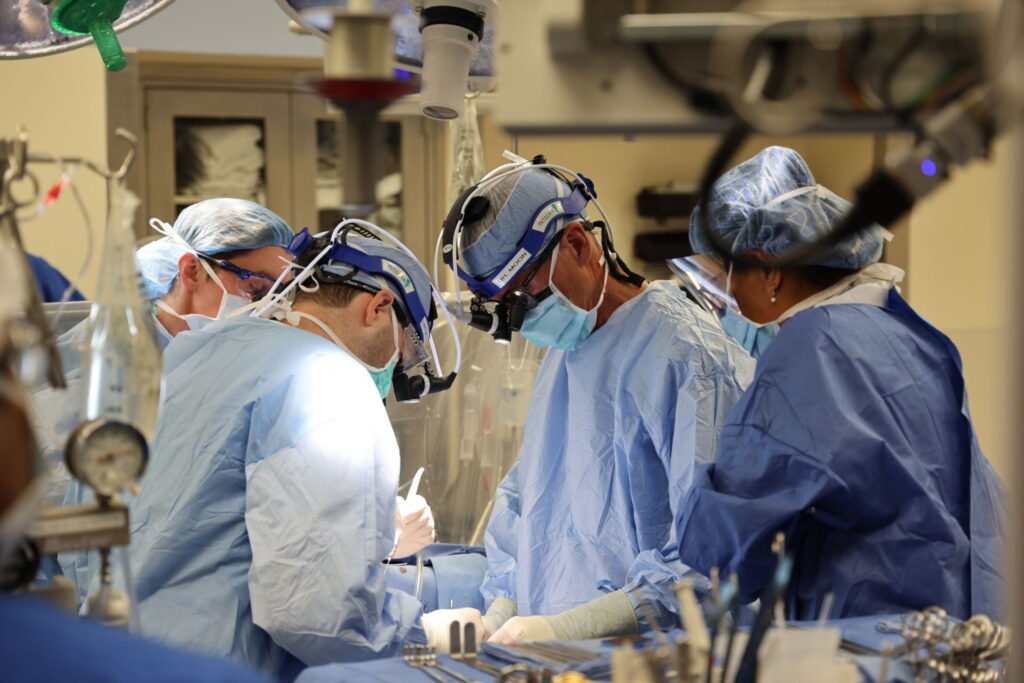
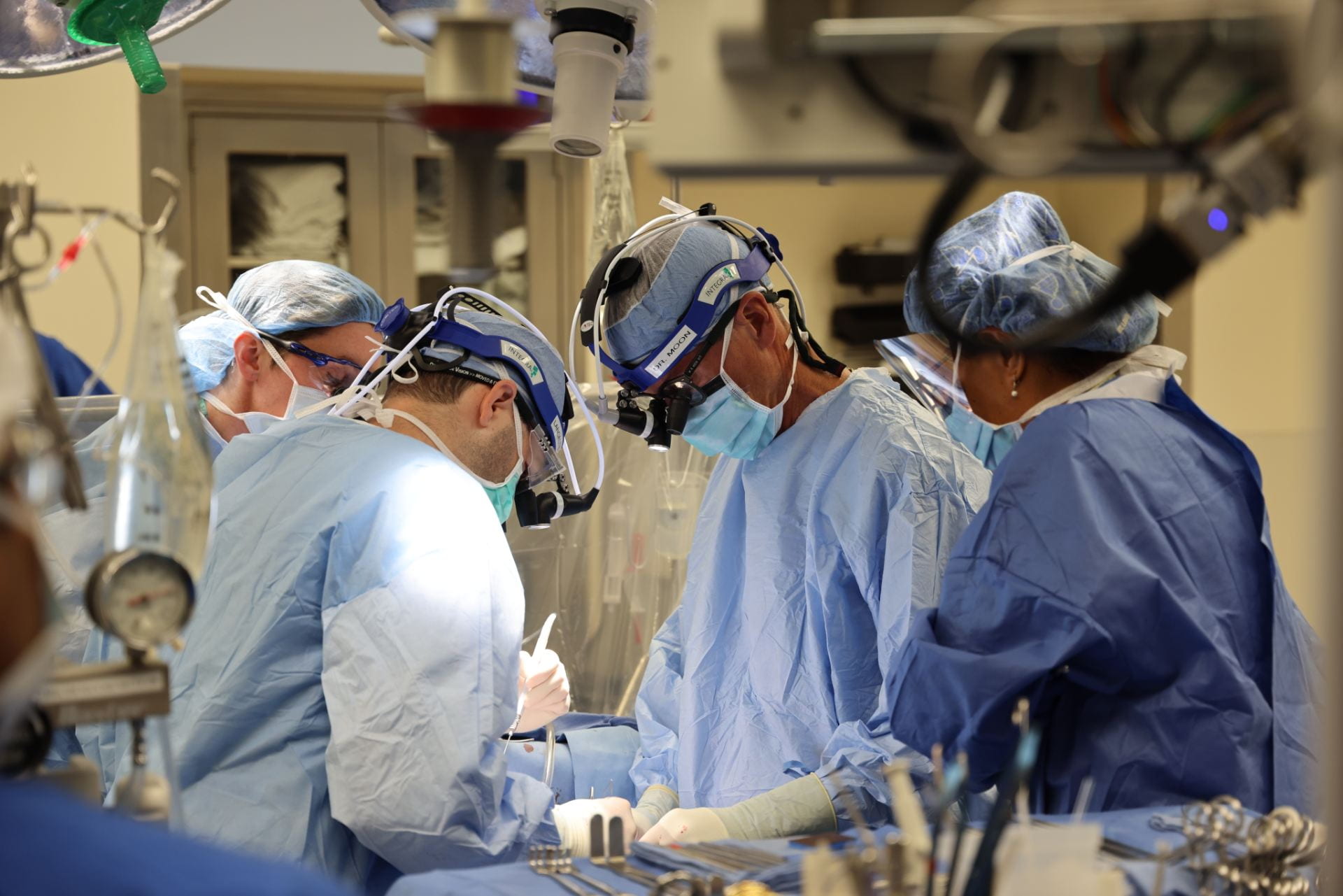
Surgeons in this section, as part of the only heart program in Missouri ranked in the top 13 nationally by U.S. News & World Report, are widely recognized as leaders in heart surgery. Working with cardiologists, vascular surgeons and a highly qualified, experienced nursing staff, cardiac surgeons offer the latest advances in technology and innovative therapies. They also employ practices supported by scientific evidence as they strive to achieve the best possible outcomes in patients undergoing heart surgery.
Section of Cardiac Surgery | 2020 Annual Report
In this unprecedented year, surgeons played a critical role in treating patients with COVID-19. Cardiothoracic surgeons typically treat conditions
of the heart and lungs, but the pandemic presented a unique problem: a deadly virus that could affect both organs and required extreme caution to protect health care workers from infection. Cardiac surgeons Akinobu Itoh, MD, PhD, Kunal Kotkar, MD, and Muhammad Faraz Masood, MD, met this problem head-on, with a commitment to do whatever it takes for their patients.
“The differences between COVID and flu or pneumonia patients start with the preparation,” Masood says. The necessary personal protective equipment and limitations on personnel in a COVID-19 intensive care unit (ICU) changed how this type of care looked from the very beginning. Normally, a team including surgeons, intensivists, infectious disease doctors and nursing staff would all be in the room with an ECMO patient. The interactions with COVID patients on ECMO, Masood says, are more critical and intense. This team still provides the same critical care, but surgeons shoulder a significant burden to limit the rest of the team’s exposure.
Extracorporeal membrane oxygenation (ECMO) provides COVID-19 patients the chance to rest their heart and lungs when the organs are failing. ECMO acts as a heart and lung for the patient, taking blood from the body, oxygenating it and pumping it back into the body at about six to eight liters per minute. ECMO was originally invented to care for pediatric patients with lung failure, but was rapidly adopted for both congenital and adult patients whose organ failure did not improve with traditional methods.
ECMO is an intensive form of therapy that requires a multidisciplinary team and high-level nursing care. Few institutions nationwide have the resources and ability to provide this care. ECMO is considered an evolving field in cardiothoracic surgery, and has seen significant growth at Washington University School of Medicine in St. Louis over the past three years. This year, over 200 people, including COVID-19 and non-COVID-19 patients, were placed on ECMO at the School of Medicine.
“Unlike flu or pneumonia, COVID affects the entire body,” Masood says. “It can have its own effects on the lungs, heart and immune system.”
COVID-19 affects different patients in different ways. In every case, the emotional toll is significant. A typical flu patient might need ECMO for about two weeks. ECMO times for COVID-19 patients can be much longer. During that time, the team is there for them through the long hours, sometimes late into the night. When the surgeons finally leave the hospital, they have to isolate from their families, living in basements or RVs to protect their loved ones. The willingness of Itoh, Kotkar and Masood to show up every day, despite the uncertainties and challenges, has been vital to delivering the highest quality care to the sickest of COVID-19 patients.
“The ability of our clinical faculty to pull together, problem solve and rise to the occasion has resulted in superb patient care,” says Timothy Eberlein, MD, the William K. Bixby Professor & Chair of the Department of Surgery. “We have been ahead of the curve in caring for the sickest COVID patients in our ICU thanks to the innovation and commitment of our faculty.”
2020 Highlights



CLINICAL
RESEARCH
EDUCATION
Cardiac Surgery Chief Marc Moon, MD, became President of the American Association of Thoracic Surgeons (AATS) in 2020. Founded in 1917, the AATS is an international organization dedicated to advancing cardiothoracic surgery. At the 100th Annual Meeting of the AATS, held virtually in April, Moon became the seventh Washington University surgeon to lead the AATS. In his President’s Message, Moon calls on cardiothoracic surgeons to address gender and racial inequality in medicine: “Let’s pledge to lead the way in cardiothoracic surgery as Hippocrates outlined 2,400 years ago with beneficence, integrity, respect for patients, mentors, and mentees, and personal and professional virtue in our quest for social justice.”
The International Registry of Acute Aortic Dissections (IRAD) is a consortium of research centers, including Washington University School of Medicine in St.
Louis, evaluating the current management and outcomes of acute aortic dissection. Cardiac surgeons and cardiovascular physicians are reviewing the database of aortic dissection cases at the School of Medicine, studying dates and times of symptom onset, presentation, diagnosis, hemodynamic signs of aortic dissection, initial and chronic medical therapy, diagnostic imaging chosen and surgical and medical management. This comprehensive study of IRAD data aims to identify new breakthroughs in diagnosis and treatment of this potentially life-threatening condition.
Richard Schuessler, PhD, Director of the Cardiac Surgical Research Laboratory, retires after an accomplished 35-year career at Washington University. Schuessler’s research focused on surgical treatment of cardiac arrhythmias, and his contributions were instrumental in the development of the Cox-Maze procedure—the first cure for atrial fibrillation. As laboratory director, Schuessler also served as a teacher and mentor for the many students, residents and research fellows who have worked in the Cardiothoracic Surgery Research Laboratory over the years. “It’s been a wonderful career,” Schuessler says. “I hope my legacy is all of the people we have trained over the years. I’ll miss the people most of all.”
Diseases of the aorta are insidious, life-threatening problems that require complex,
high-level care. The aorta is the main vessel that sends blood from the heart to the body. Aortic dissection occurs when the wall of the aorta tears, blocking or diverting circulation and reducing the amount of oxygen and nutrients that reach vital organs. An aortic aneurysm is a balloon-like enlargement in the aorta, difficult to detect but deadly when ruptured.
Cardiac Surgery Section Chief Marc Moon, MD, and cardiac surgeon Puja Kachroo, MD, treat patients with even the most complex aortic pathology. These complex conditions are often related to hypertension, inflammatory conditions, familial history or genetic connective tissue disorders including Marfan syndrome and Loeys-Dietz syndrome.
“Aortic dissection is often fatal when missed,” Moon says. “But with proper education, physicians know what signs to look for. The patient might feel like they are having a heart attack or stroke. Chest pain is the number one symptom for aortic dissection.”
The Department of Surgery has a longstanding history of excellence in the care of patients with aortic disease. Moon, the director of the Center for Diseases of the Thoracic Aorta (CDTA), has performed complex aortic surgery for over 20 years. Kachroo, who joined the faculty after completing a fellowship in the Cardiothoracic Surgery Section in 2016, has expanded the number of cases treated at the CDTA and introduced minimally invasive cardiac procedures for valve replacement and coronary bypass. Moon and Kachroo work closely with vascular surgery colleagues and a multidisciplinary team to coordinate the evaluation and management of patients.
“It takes a lot of experience to deal with high-risk aortic patients,” Kachroo says. “I have been fortunate to have Dr. Moon as a mentor and teacher. His experience has been very helpful in expanding my abilities, one step at a time. He was one of the earliest adopters of valve sparing aortic root replacement, a very complex and difficult to learn operation. Luckily, I learned from him as a fellow and can continue to build on this practice. With the two of us doing these complex aortic surgeries, we can truly treat the gamut of aortic disease.”