St. Louis Children’s Hospital is the largest children’s hospital in the region, with nearly 400 licensed beds and an American College of Surgeons-verified Level I pediatric trauma center. It offers comprehensive services in every pediatric medical and surgical specialty and is recognized as one of America’s top children’s hospitals by U.S. News & World Report, which in 2020 ranked the hospital in all 10 specialties surveyed.
St. Louis Children’s Hospital | Department of Surgery 2020 Annual Report
Patients with congenital heart disease often have rare, complex heart defects. These conditions present challenges for preoperative planning, trainee education and patient counseling. It can be difficult to describe a heart defect to a patient or their family. Cases of rare congenital cardiac problems may not arise during a fellow’s training. Developing innovative methods of treating these conditions requires a simulated environment for surgeons to practice new techniques outside of the operating room.
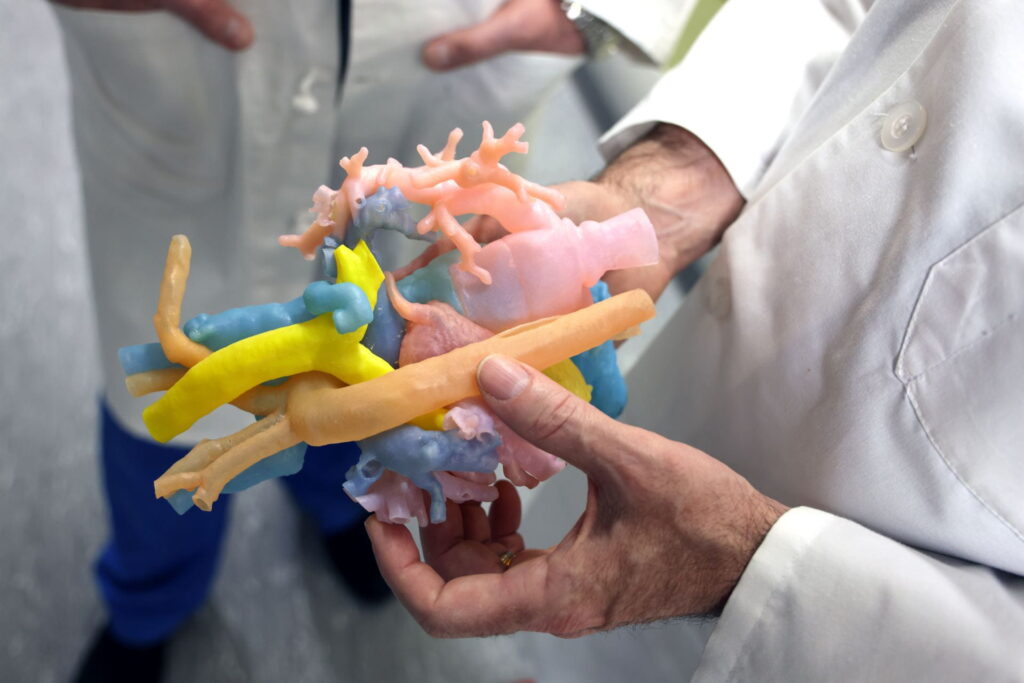
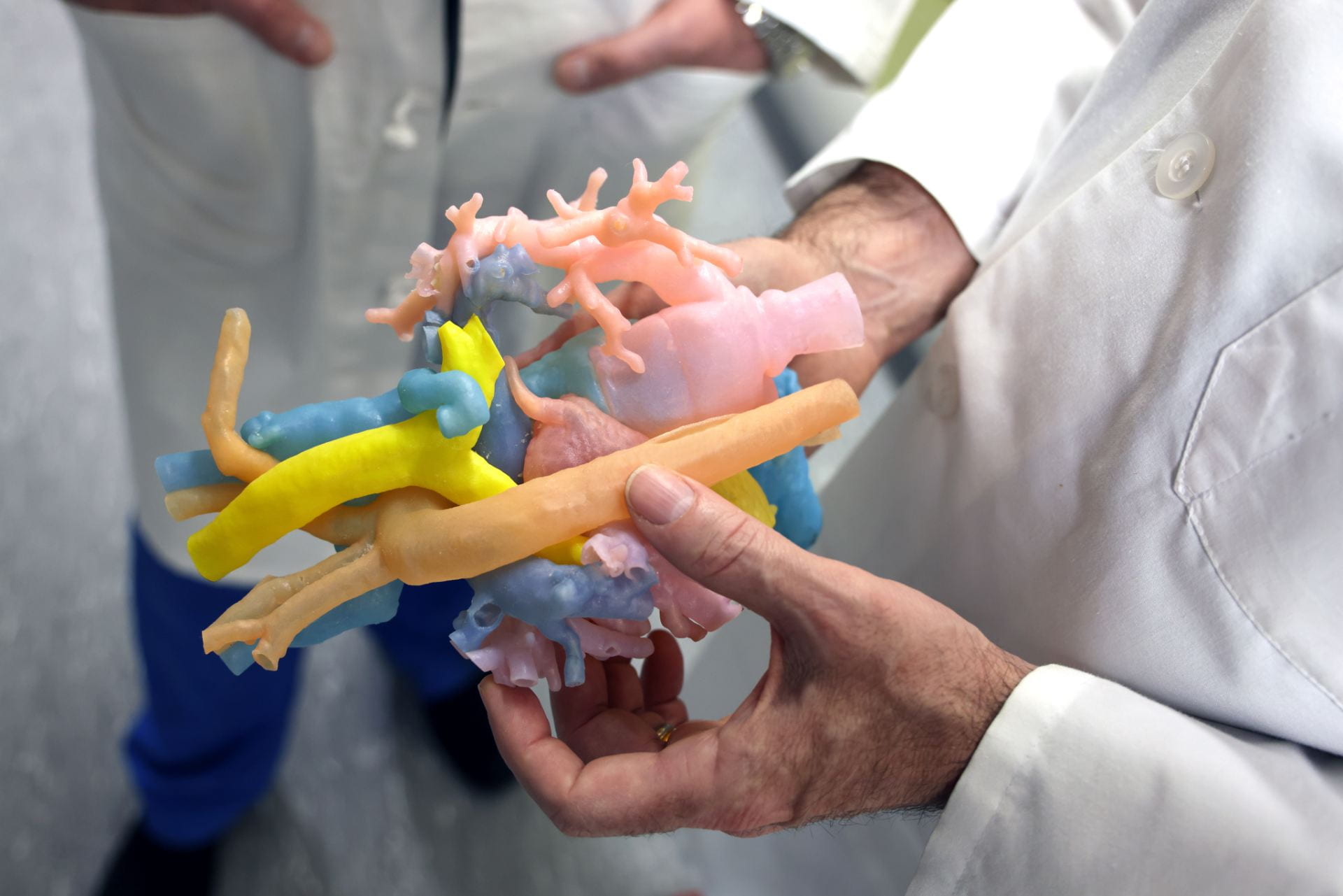
Surgeons in the Section of Pediatric Cardiothoracic Surgery have found 3D printing to be a transformative technology for preoperative planning and surgical simulation in congenital heart disease. Printing models of the heart allows the surgeon to plan for a procedure, teach trainees in a safe simulated environment and, importantly, educate patients and families.
“It’s quite helpful,” says Section Chief and Cardiothoracic Surgeon-in-Chief at St. Louis Children’s Hospital Pirooz Eghtesady, MD, PhD. “Some of the hearts we’re working with are the size of a strawberry. When you talk to the family and you can show them why this is a complex operation, I think it helps them have a better understanding of what we are doing.”
Eghtesady describes congenital heart surgery as being like rebuilding a house. With 3D-printed hearts, surgeons can move pieces to practice this process, connecting arteries and vessels, rebuilding valves.
Three-dimensional models have also played a role in surgical training. In addition to allowing practice on highly accurate simulators, the 3D models expose trainees to pathological features they may rarely encounter. Future congenital cardiac surgery fellows will have the opportunity to practice an index of rare, complex operations on 3D-printed hearts, preparing them to help a wider spectrum of cardiac patients after training.
“This technology also allows us to think differently and develop new operations for some of themost complex congenital problems,” Eghtesady says. “The cornerstone of our section has been innovation. My mission statement is to make it a better world for families that need our help, one innovation at a time.”
2020 Highlights
CLINICAL
As director of liver transplant at Barnes-Jewish Hospital and St. Louis Children’s Hospital, Maria B. Majella Doyle, MD, MBA, leads the Pediatric Liver Care and Transplant Center team in performing transplants for children with acute liver failure, liver cancers including hepatoblastoma and hepatocellular carcinoma, and metabolic disorders. In the past year, the center has introduced domino liver transplant for patients with maple syrup urine disease. Domino liver transplant takes a liver that does not work for one person due to metabolic disorder, and transplants the liver to a person without that disorder. The Pediatric Liver Care and Transplant Center provides comprehensive evaluation, treatment and care for children with all forms of liver disease.

RESEARCH
Research in the Section of Pediatric Cardiothoracic Surgery is at the forefront of innovation for children with congenital heart and lung conditions. In the past year, researchers from the section, in collaboration with colleagues from across the School of Medicine, have published several peer-reviewed articles covering the breadth of pediatric cardiothoracic surgery. The section is highly active in research studies involving ventricular-assist devices in bridging children to lung transplantation. Researchers recently received an Innovative Project Award from the American Heart Association for research related to the role of maternal gut virome in the development of congenital heart defects.

EDUCATION
The Pediatric Surgery Fellowship is among the most sought-after training programs in the country, with over 100 applicants each year vying for a single position. Division Chief Brad Warner, MD, has seen a rise in the number of general surgery residents pursuing fellowship training in pediatric surgery in recent years. In response to this growing interest, the division is developing a program to fast-track general surgery residents interested in pediatric surgery early in their residency. Nearly half of the program’s fellows have been women, exceeding national averages. “As a division,” Warner says, “We have worked to develop an inviting and engaging experience for all pediatric surgery trainees, from medical students to residents and fellows.”
The Pediatric Colorectal Center at St. Louis Children’s Hospital and Washington University School of Medicine in St. Louis brings together multidisciplinary pediatric experts to provide high- quality care to children with complex colorectal issues like Hirschsprung disease and anorectal malformations. Using state-of-the-art technology, top expertise, multidisciplinary care and goal-setting, the Pediatric Colorectal Center provides personalized solutions to improve the quality of life for children and their families.
Pediatric surgeon Baddr Shakhsheer, MD, established the center to help children like Savannah, who was born with a rare chromosomal deletion that caused several serious health problems, including cerebral palsy, seizures, kidney and heart disease, a compromised immune system and complex bladder and bowel issues. Savannah underwent testing at the Pediatric Colorectal Center, and her family talked with Shakhsheer about their goals and the best solution for their daughter. Ultimately, Savannah had surgery to address her hypofunctioning colon.
“These are serious problems that have lifelong implications,” Shakhsheer says. “In pediatric colorectal care, you’re entering into a long-term relationship with the family. You see them not only for the surgical procedure, but through the postoperative management as well.”
The program at the Pediatric Colorectal Center offers a comprehensive approach to management and treatment of patients with gastrointestinal problems. The team includes gastroenterology, radiology, rehabilitation, nursing and surgery. Patients receive complete evaluation and diagnostic workup, including motility testing, manometry, imaging and pathology, as well as top pediatric care, all at St. Louis Children’s Hospital.
“Dr. Baddr Shakhsheer has been such a blessing,” Savannah’s mother says. She describes him as a gentle giant. “He is very honest and straightforward. He’s smart and dedicated to his profession. Most importantly, he wants to make every child feel so much better.”
Shakhsheer completed general surgery residency at the University of Chicago. He joined the faculty after completing the Pediatric Surgery Fellowship at Washington University and St. Louis Children’s Hospital. Shakhsheer is well-versed in both traditional and minimally invasive approaches to colorectal surgery, and is driven to provide the best possible care to pediatric patients.
“It’s a joy and a privilege to work with children,” he says. “There’s no other way to say it.”