Surgeons in this section offer open and endovascular treatment for vascular diseases. Surgeons also participate in clinical trials of stent graft devices to treat thoracic aneurysms using endovascular techniques. Vascular surgeons provide clinical training in residency and fellowship programs accredited by the Accreditation Council for Graduate Medical Education. Numerous general surgery residents also rotate on the service. Members of the section lead research in basic science, translational research, clinical outcomes and novel device trials.
Section of Vascular Surgery | 2020 Annual Report
Vascular surgeon-scientist and Director of the Vascular Surgery BioBank Mohamed Zayed, MD, PhD, is leading multiple NIH-funded research projects to develop effective new treatments for patients with peripheral arterial disease (PAD) and other vascular diseases.
The Zayed laboratory is studying why diabetic patients are at significantly higher risk of developing PAD, which causes plaque buildup to block blood flow to the extremities and can lead to serious complications such as wounds and amputation. In a recent study, the Zayed lab discovered a protein present in patients that are more prone to PAD and carotid artery disease.
“Our hypothesis is that this molecule actually makes LDL, what we would call ‘bad’ cholesterol,” Zayed says. “This could be groundbreaking, because rather than targeting LDL, we could target that molecule, which ultimately affects a person’s risk of atherosclerosis.”
For this research, Zayed received the Academy of Science—St. Louis 2020 Innovation Award at the 26th Annual Outstanding St. Louis Scientists Awards.
Current treatments for PAD are primarily focused on bypassing the blockage, but do not directly address the disease on a molecular or biological level. Zayed is studying a molecular probe that would allow surgeons to image atherosclerosis in the arteries and diagnose and extract plaques before they grow or rupture. The BioBank has collected over 10,000 vascular specimens, providing a rich repository for this molecular research.
“In addition, we are recruiting patients in a clinical trial to administer this probe preoperatively and extract the plaque,” Zayed says. “We are taking this from bench to bedside for patients, then back to the bench with the extracted plaque for further study.”
Zayed’s vascular innovation research, in collaboration with the McKelvey School of Engineering, has led to the development of a thrombectomy catheter that may be a safer, more efficient and effective method of removing large clots that could be deadly if left untreated. The catheter is a multimodal mechanism capable of mechanical and chemical lysis and suction thrombectomy. The Zayed lab and industry partners are seeking FDA approval for clinical use of the catheter.
“None of this work would have been possible without the ingenuity, creativity and hard work
of the team of scientists, engineers and support staff that I have the fortune to work with on a daily basis,” Zayed says. “I am truly blessed to work with an amazing team that not only makes it enjoyable to come to work, but also makes our research enterprise successful and productive.”
2020 Highlights
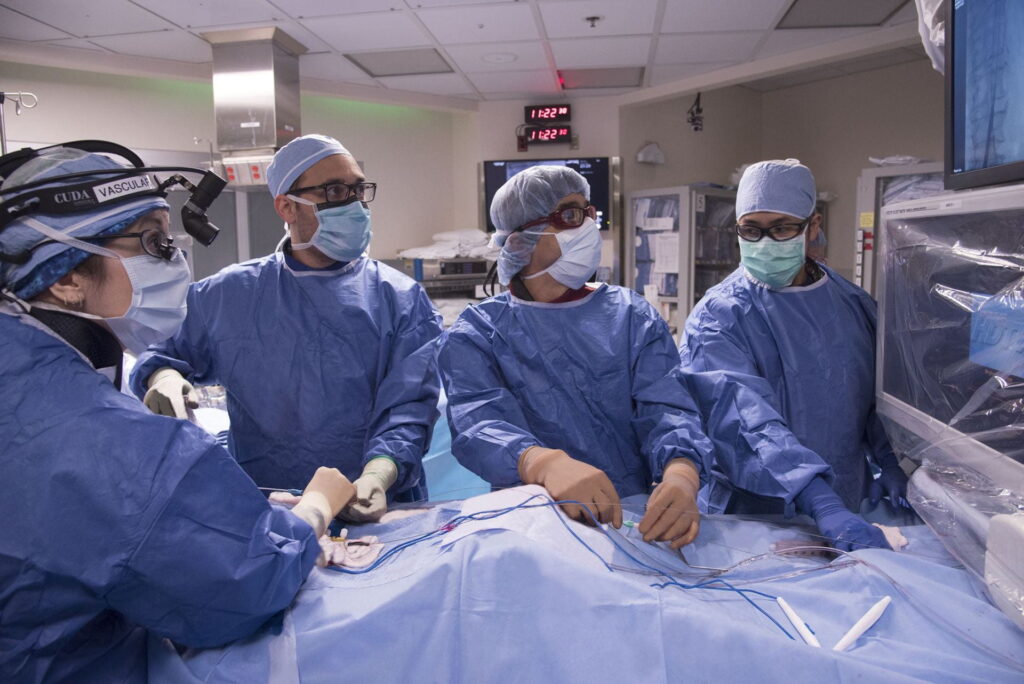
CLINICAL
The Department of Surgery is developing a multidisciplinary, team-based care program for patients with limb complications from diabetes and peripheral vascular disease. These conditions reduce circulation, making it more difficult for soft tissue wounds to heal, ultimately leading to foot or leg amputation for many patients. Section Chief Luis Sanchez, MD, and vascular surgeons Patrick Geraghty, MD, J. Westley Ohman, MD, and Vipul Khetarpaul, MD, are coordinating with plastic and reconstructive and acute and critical care surgeons to offer limb preservation procedures to this formerly underserved patient population who might otherwise require amputation.
RESEARCH
Abdominal aortic aneurysm (AAA) rupture can be life- threatening and often affects people who are not good candidates for open arch repair due to other health problems. Over the last year, the Vascular Surgery Section has significantly increased endovascular options for treating these patients to prevent AAA rupture. Washington University School of Medicine in St. Louis is participating in numerous clinical trials on the management of aortic pathologies. Vascular surgeon Sean English, MD, received an RO1 grant from the NIH for his research of targeted molecular imaging and treatment of AAA.
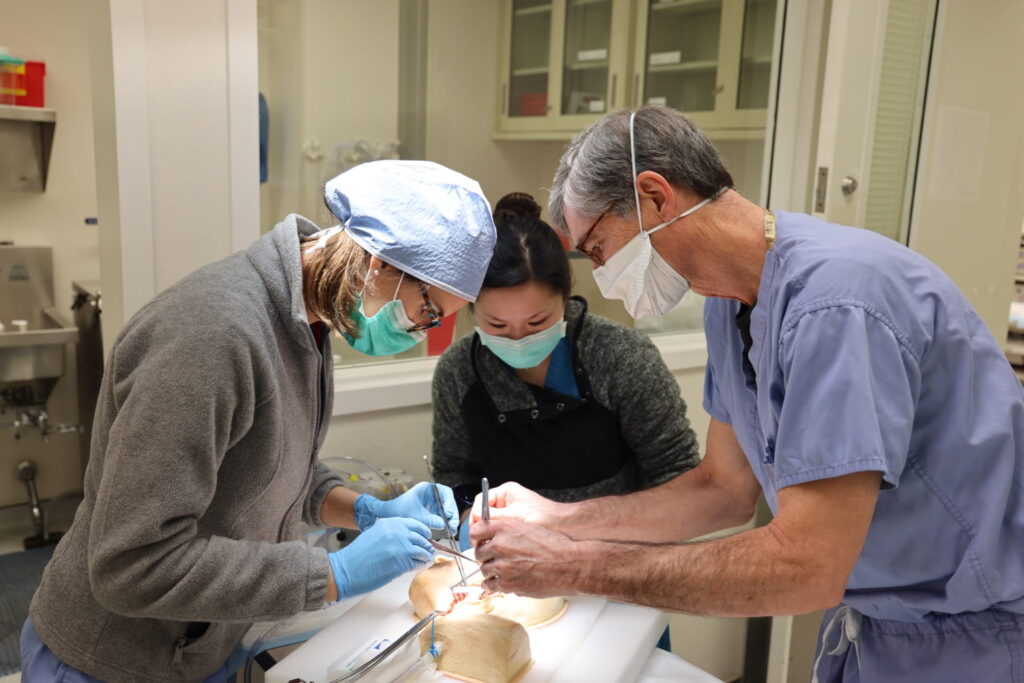
EDUCATION
The Vascular Surgery Section offers both a two-year Fellowship Training Program, which began in 1986, and an Integrated Residency Program, which enrolled its first resident in 2012. The vascular training programs share a common goal to train surgeons who wish to focus exclusively on vascular and endovascular surgery and the management of patients with vascular disease. “The vascular surgery programs are currently training our largest complement of residents and fellows,” says Section Chief Luis Sanchez, MD. “Our trainees continue to excel in open and endovascular procedures and diagnostic imaging for patients with vascular disease, participation in meetings and conferences, and involvement in research efforts.”
New technologies and techniques available at Washington University School of Medicine in St. Louis allow vascular surgeons to manage patient populations with complex problems who previously had few or no good treatment options.
Deep vein thrombosis (DVT) is a serious condition that develops when a blood clot forms in one
or more deep veins, usually in a person’s leg. The Centers for Disease Control and Prevention estimate that one third to one half of people who develop DVT will have long-term complications. The worst complication of DVT, pulmonary embolism (PE), is often fatal.
In the past year, vascular surgeons Gerald Fortuna Jr., MD, Col, USAF, SFS, MC, MBA, and J. Westley Ohman, MD, have built a practice for the management of extensive DVT/PE using the ClotTriever Mechanical Thrombectomy System. The School of Medicine is participating in the ClotTriever Outcomes (CLOUT) Registry using this new device. The CLOUT Registry evaluates real world patient outcomes after treatment of acute, subacute and chronic proximal lower extremity DVT with the ClotTriever Thrombectomy System.
A number of new clinical trials utilizing novel devices and techniques also enable the Section
of Vascular Surgery to provide advanced aortic management to more patients with aneurysms and dissections. Abdominal aortic aneurysm (AAA) and thoracic aortic aneurysm (TAA) are life-threatening enlargements of the aorta. Aortic dissection is a rare, frequently deadly tear in the aortic wall.
Section Chief Luis Sanchez, MD, the Gregorio A. Sicard Distinguished Professor of Vascular Surgery, has led the growth of endovascular treatment of patients with complex aortic disease. Until recently, there was no endovascular option available for TAA, though many patients with the condition are not candidates for open arch repair due to the complexity of their health problems. Ongoing trials and registries allow vascular surgeons at the School of Medicine new forms of management for a variety of aortic pathologies, from the aortic arch to the distending thoracic aorta, thoracoabdominal aorta and infrarenal aorta, as well as complex juxtarenal aneurysms.
“The breadth of opportunities that we have to manage patients with complex anatomy and complex problems, who are at high risk for standard open surgeries, has grown significantly,” Sanchez says. “We have access to new devices and trials unmatched by other local and regional centers, allowing us to manage a population of patients who may have had no good options in the past.”


