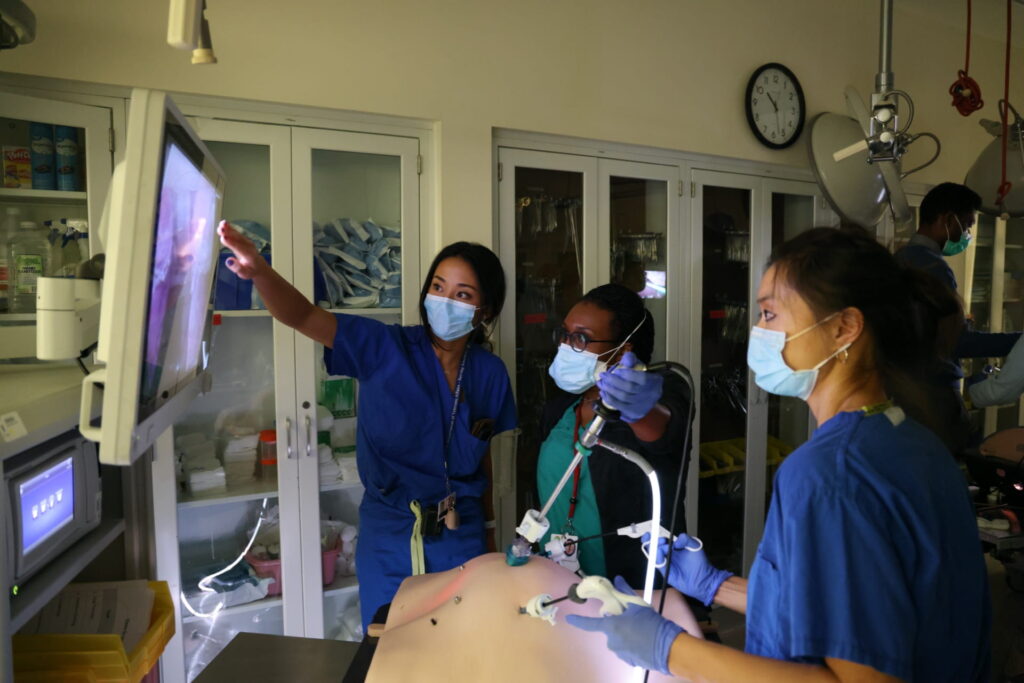
Each year, the Washington University Institute for Surgical Education (WISE) Center welcomes a new group of interns with a surgical skills “boot camp,” cultivating important fundamentals such as suturing, knot tying and laparoscopic techniques. Throughout the year, other labs explore important operative skills for trainees at all levels. Social distancing and COVID-19 restrictions present particular challenges for surgical training this year, but the WISE Center has met those challenges with solutions that continue to innovate in the world of surgical education.
Interns this year participated in a mostly remote boot camp by taking home Ethicon laparoscopic trainer boxes, training instruments and suture materials. Normally this training would take place in-person, with a coach and intern practicing the skills together. A built-in webcam on each Ethicon trainer made it possible to simulate this experience while interns safely practiced skills from their homes.
“We were able to livestream with interns as they did their training,” says Michael Awad, MD, PhD, Director of the WISE Center. “The coach would also have a trainer box with a webcam, so we were able to do the skills training as if we were standing side by side.”
Other skills labs were more difficult to conduct remotely. Once WISE was able to safely reopen, carefully aligning with state and federal guidelines while still offering world-class surgical simulation training, the staff scheduled these labs over an extended period to reduce the number of trainees on site at any one time.
The first of these labs, the COVER wound management lab, helps trainees to select the best products to use for different types of wounds and learn how to properly apply them. The COVER lab addresses common causes of soft tissue injury and infection; obstacles to closure; vacuums, chambers and more; epithelialization; and rationale for different wound care materials. Surgical Skills Coordinator Angie DeClue describes this lab as very tactile: residents must feel how to apply pressure or notice any problems like an air leak in a machine.
The next in-person lab was an opportunity for all residents—from interns to chiefs—to practice their skills. The SAVE (surgery for abdominal/thoracic violence) trauma lab is a chance for residents to collaborate and develop comradery across the board while also developing vital operative skills, as more senior residents train junior residents. The lab includes simulation practice for less invasive procedures such as laparotomies, as well as experience with small bowel resections, diaphragm injuries and splenectomies.
“These are excellent cases for senior residents to lead on with junior residents,” Awad states. “It exemplifies their teaching and communication abilities as they guide junior residents through the procedures.”
The lab then moves into more complex aortic and cardiac procedures, which provide a chance for attending surgeons to mentor chief residents.
“To keep everyone safe and socially distant, we started these labs earlier in the year,” Peggy Frisella, Administrator of WISE and Manager of Research Operations for the Institute for Minimally Invasive Surgery, explains. “What we found was that residents liked to hit the ground running with this experience in trauma. We are learning about opportunities to schedule our labs differently in future years, even after COVID-19.”

The WISE Center’s trainees also include OR staff and surgeons seeking to expand their surgical skills. Awad has extended this group of trainees to include surgeons across the country who want to learn robotic surgery. In the past, these surgeons would visit St. Louis to learn skills from Awad, then he would join them at their institution to proctor and coach them through their first robotic procedures.
With help from Intuitive Surgical, a da Vinci system is available in the WISE Center, allowing for weeks of training at a time and the establishment of a remote training program for surgeon education. A surgeon can participate in remote training with Awad, then receive the same proctoring experience virtually, as Awad is able to see what the surgeon sees through their robotic console. This “telementoring” or “teleproctoring” technology allows him to communicate directly with the surgeon, highlight anatomy on the monitor and make recommendations in real-time.
“It’s like WISE without walls,” Awad says. “It allows us to expand our boundaries beyond our normal population and think about how we can teach trainees that might not otherwise have had the opportunity to come to the St. Louis area.”