Helping people is Carmen Lake’s life’s work. She volunteers at her church and has volunteered with her local schools and community organizations, and serves as case worker and caregiver for her three children with special needs. “There’s nothing better than making a positive impact on someone’s life,” Carmen says. For nearly two decades, Carmen struggled with a medical condition that in recent years has made using her hands nearly impossible. Now she wants to help people with similar conditions get their hands, and lives back.
Years ago, Carmen was diagnosed with scleroderma, a rare chronic disease that involves the hardening and tightening of the skin, as well as problems with the vascular system. Scleroderma affects people in different ways. Some people develop areas of tight skin around their face and mouth. Others have problems with their heart, lungs or other organs. Carmen’s problems have greatly impacted the use of her hands and fingers. Carmen’s hands turned white and became sensitive to cold. This common early symptom of scleroderma is known as Raynaud syndrome. This problem was compounded by the development of blockages within her arteries which caused the pain to change from intermittent to persistent and severe.
“The pain was constant and made everything so much more difficult,” Carmen says. “You can’t grip, you can’t pinch, you can’t do anything. There’s just this constant pain that goes straight to the bone.”
Open sores, called digital ulcers, formed on Carmen’s fingers. These painful ulcers, caused by damage to the blood vessels in her arm and fingers, took months to heal. Some ulcers did not heal at all. While some of her fingertips developed bone infection and required amputation, others simply vanished due to bone resorption from impaired blood flow. Carmen was in pain, and losing function fast. She knew she needed help.
Finding a Solution
“When I first met Carmen, she came in with a very clear picture of insufficient blood flow. Her fingers were ischemic and contracted, which is typical of scleroderma. Even with maximal therapy and multiple hospital admissions, she still had insufficient blood flow and nonhealing ulcers,” says Mitchell Pet, MD, who directs the hand surgery program at Washington University Plastic and Reconstructive Surgery. “Digital pressure studies showed very poor blood pressure in her fingers, and an angiogram showed that both her radial and ulnar arteries were blocked along long segments. She was on the path to losing her hand.”
Scleroderma treatment often involves moisturizing the affected skin, performing physical therapy and taking medication as prescribed. Most patients begin by seeing a rheumatologist, who can develop a treatment plan to manage symptoms and slow disease progression. Carmen tried it all—but despite all of this she continued to have painful wounds and progressive tissue loss.
Fortunately, Carmen was referred to Dr. Pet, a fellowship-trained, board certified Washington University hand surgeon with a focus on microvascular and reconstructive surgery. Dr. Pet specializes in hand surgeries involving even the smallest vessels.

The most traditional surgical treatment for blocked arteries would be angioplasty, which opens up the blocked arteries to restore blood flow, usually with a minimally invasive approach. The problem with angioplasty for someone in Carmen’s situation, Dr. Pet explains, is that the arteries in the hand are usually too small and too clogged. Another option Dr. Pet considered was arterial reconstruction—replacing a blocked area of artery with a grafted vein or artery from another part of the body.
“Carmen was not a candidate for reconstruction of her native arterial tree for a few reasons,” says Dr. Pet. “Her arteries were occluded along very long segments. Her scleroderma had caused vascular damage not only in the arm, but in the fingers and hand. Even if we could get blood to flow through the arteries her arm, there was nowhere for it to go once it got to the hand. We had to find a different way for blood to reach her fingertips.”
In a typical circulatory system, blood pumps from the heart to the rest of the body through arteries, then returns to the heart through veins. Carmen’s scleroderma had caused severe arterial blockage, but left her veins functioning normally. Dr. Pet proposed arterialization of the venous system. This uncommon but well-described procedure reverses the flow of the venous system. Instead of returning blood from the fingers, selected veins are recruited to deliver oxygen-rich blood to the fingertips when the arterial system can no longer do so.
Simply put, Dr. Pet recognized that Carmen’s arteries were not recoverable, so he provided her blood an alternative route to the fingertips.
Working for Results
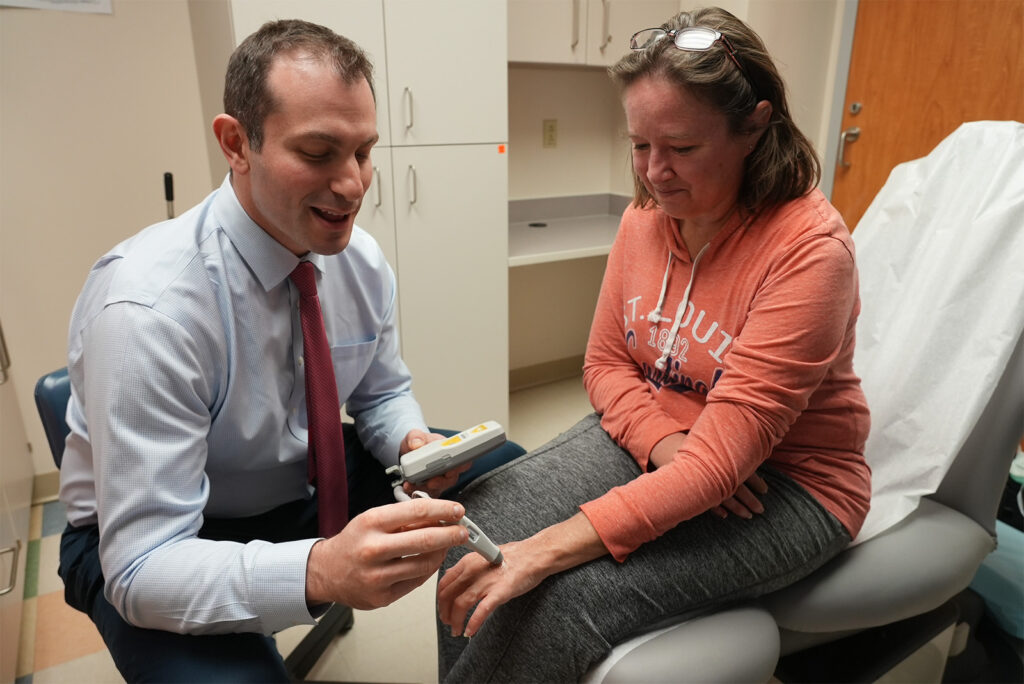
After the arterialization procedure, Dr. Pet and Carmen noticed some immediate changes. Carmen’s hand went from cold and pale to her normal skin color before she even left the operating room. Using a Doppler ultrasound, Dr. Pet could hear a strong, steady pulse in Carmen’s hand, where there was none before. These were early indicators that the vein-turned-artery was pumping freshly oxygenated blood into the hand and fingers.
Other results took more time. Carmen’s ulcers healed gradually now that they had the circulation necessary for wound healing. There was some pain the first night after surgery as her usually-starved tissues encountered blood flow again, but Carmen says it was worth it for the results she has achieved. Today, she has no pain or wounds, and had no painful reaction to the cold. She can use her hand without the constant worry and discomfort that plagued her for years.
“Before the surgery, I couldn’t leave the house without gloves or handwarmers. Even in the summer, I had to use a steering wheel cover because it hurt to touch the leather. Little things, like holding a cup, were hard to do even somewhat normally. You can’t get away from the pain, not even to tie your own shoes,” Carmen says. “From before to after surgery, it’s night and day. I can move again. I’ve taken up gardening. I feel like I have the chance to reinvent myself thanks to Dr. Pet and my physical therapists.”
Hand therapy after surgery is critical to achieving results like Carmen’s, Dr. Pet says. The surgery improved her blood flow, but it took time and dedication for Carmen to regain the mobility and function she has today. Dr. Pet and the team of Washington University plastic and reconstructive surgeons work closely with therapists at the Milliken Hand Rehabilitation Center at Barnes-Jewish Hospital to provide comprehensive care for their patients.
Making a Difference
Carmen’s first arterialization, on her left hand, took place in early 2021. When her right hand started to show some serious problems the following year, Carmen immediately called Dr. Pet.
“It’s very rewarding when a patient tells you they are happy with their results after surgery, but Carmen really showed she meant it when she came back to have the same procedure on the other arm. That’s a good sign that you’ve really made a difference,” Dr. Pet says.
Dr. Pet notes that Carmen was a great patient to work with because she articulated her goals and concerns and she provided honest, constructive feedback. He encourages patients to take an active role in their treatment and recovery process.
“For her second surgery, and the therapy after, we were able to make some refinements based on Carmen’s feedback. Building these relationships with patients helps you continue to grow and develop as a surgeon,” Dr. Pet says.

Dr. Pet also emphasizes that no treatment is “one size fits all.” Arterialization was appropriate for Carmen, but other patients with vascular disease may benefit from arterial reconstruction or other procedures.
Now Carmen wants to advocate for others with scleroderma and other upper extremity vascular diseases.
“I hope this will help more people with conditions like mine,” Carmen says. “I know I was close to losing a hand. I was losing life as I knew it. Dr. Pet absolutely saved my way of life. If there were options for me, there might be options for other people in similar situations.”
Learn more: Washington University Plastic and Reconstructive Surgery