Assistant Professor of Surgery Kelly Currie, MD, is a surgeon in the Division of Plastic and Reconstructive Surgery and sees patients at Christian Hospital and Alton Memorial Hospital. She specializes in hand, upper extremity and general reconstructive plastic surgery. Her medical journey brought her to plastic and reconstructive surgery because of her desire to give patients immediate results. “I chose to become a surgeon because I like instant gratification and fixing things,” says Currie. “For plastic surgery, I like the fact that I can operate on any part of the body, and I can reconstruct things and give patients a sense of normalcy.”
Part of how Currie brings normalcy to her patients is through a new technique in surgery, known as Wide Awake Local Anesthesia No Tourniquet, or WALANT. This technique is changing the hand surgery field, and in many cases, it is better for patient experience and outcome, the surgeon using the technique and the hospital.
“I would like to see this WALANT surgery really take hold at all Washington University School of Medicine locations and increase the number of surgeries and various types of cases I’m doing on the hand, wrist and forearm,” states Currie. “I want it to be well-known that this technique is available for our patients.”
To make this technique more well-known, Currie answers frequently asked questions about WALANT.
WALANT: Frequently Asked Questions
What is WALANT?
WALANT stands for Wide Awake Local Anesthesia No Tourniquet and is a technique used for hand and wrist surgery procedures. The technique does not require any sedation, general anesthesia or tourniquets but uses local anesthesia medications, lidocaine and epinephrine, instead. The lidocaine blocks pain and epinephrine stops the bleeding. This allows the patient to remain fully awake during the procedure.
What are the benefits of a WALANT procedure?
WALANT procedures offer several benefits for the patient, surgeon and hospital or clinic.
The patient spends less time in the hospital or clinic because there is no need to come in two hours before surgery like patients would to prepare for surgery in an operating room. This means the patient can take less time off work and plan less time for childcare if needed. Oftentimes, there’s a possibility they can have the surgery the same day they meet with a surgeon because there is no need for preoperative testing or an operating room. It’s one less trip the patient must leave their house for, and is especially beneficial during the COVID-19 pandemic.
WALANT patients rarely experience the nausea or vomiting that is associated with general anesthesia medications. Furthermore, because the patient is awake during the surgery, they have the opportunity to know exactly how the surgery is performed. Patients can demonstrate hand function during the procedure, allowing for immediate evaluation of the treatment. This leads to less complications with postoperative rehab and can reduce time at the follow-up appointment. The WALANT technique has also been shown to reduce the postoperative opioid use for patients.
What can a patient expect before and after surgery?
Before using the WALANT technique, a surgeon will explain the anesthesia and procedure to the patient. The patient will be injected with the local anesthesia medication and may feel a little bit of burning at first, but after about a minute it is numb. After the surgery is over, since the patient has already talked to their surgeon during the surgery, the patient can expect to go home immediately.
Can you feel anything during a WALANT hand surgery?
Patients will feel the initial needle poke, no worse than an IV, which is what they would have if they had a surgery in the operating room. Some patients have said that they are able to feel that the surgeon is doing something in their hand, but they do not feel anything painful. If the surgeon has to do an additional injection in another spot, he or she will do it where there is already numbness.
Can a patient watch their surgery?
Yes, a patient can watch the surgery. Some patients like to watch so that they understand how the surgery works and can know how it is going, but a patient does not have to watch the surgery. Many will bring their phones, listen to headphones or watch a movie, so that they are completely distracted. Others like to have a conversation with the surgical team about other topics.
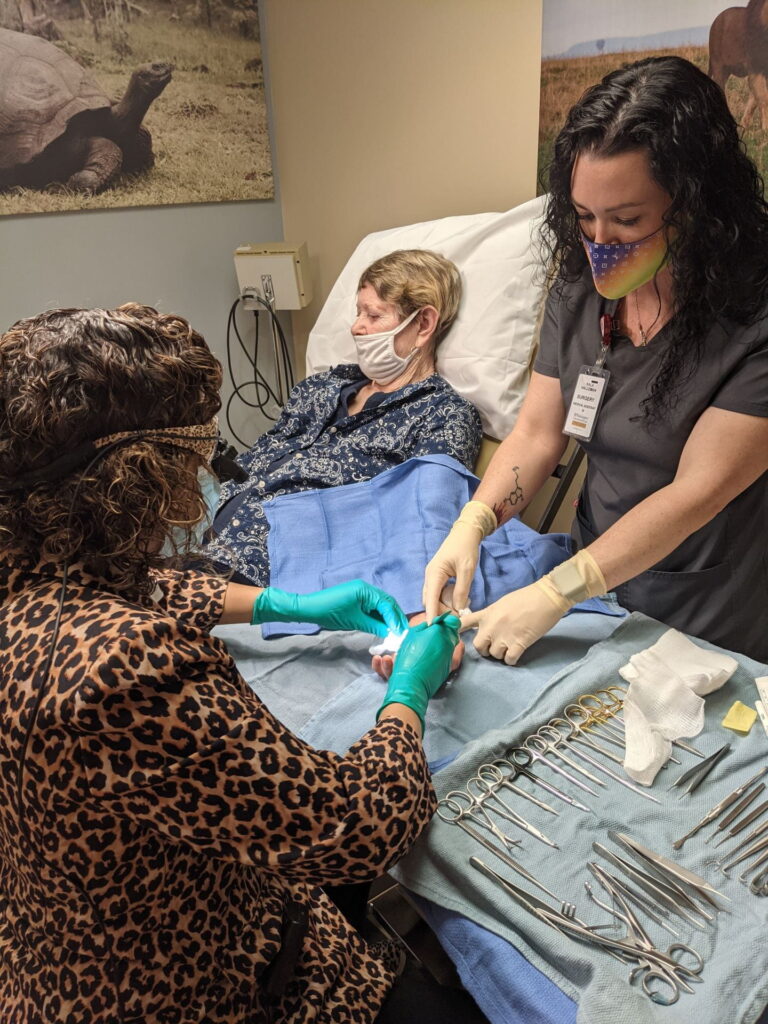
Kelly Currie, MD, left, performs surgery on Georgua Lyles, center, using the WALANT technique. 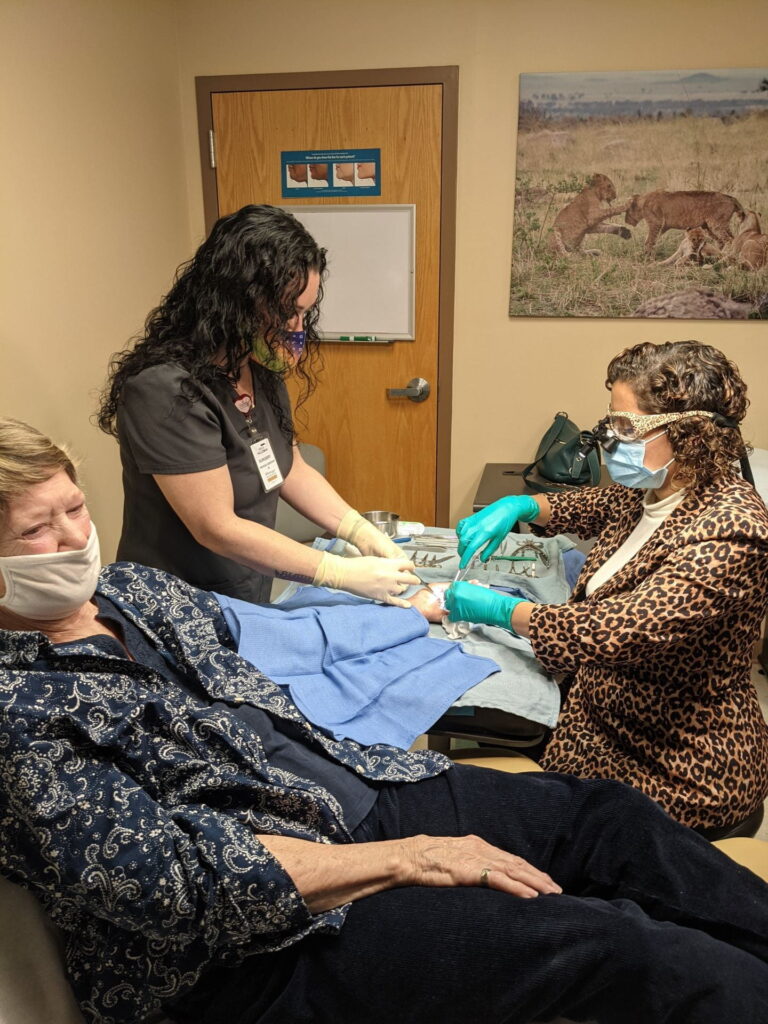
Kelly Currie, MD, right, performs WALANT surgery with the help of medical assistant, center.
Why do some patients prefer WALANT?
The WALANT technique offers a variety of benefits for patients compared to a surgery done under sedation in the operating room. Patients prefer WALANT because they do not have to fast before their surgery and are free to eat throughout the day of their procedure. Furthermore, patients do not necessarily have to stop chronic medications, such as blood thinners, before surgery. Oftentimes, this results in a much safer experience for the patient.
WALANT surgeries are also more convenient, as it takes up less time and usually allows a patient to drive home immediately, without the need for a driver. WALANT procedures are done in a reclined chair, so patients can adjust their position to remain comfortable during the surgery.
Moreover, patients prefer WALANT because they feel like they have more time with the surgeon and can ask them questions while it is happening. This leads to more patient satisfaction overall.
Is everyone a candidate for WALANT?
While WALANT is a great option for many patients, not everyone is a candidate for this type of procedure. Though it is normal to be nervous, people who are not good candidates are those who are very anxious and may not be able to cooperate with instructions. Other patients who would not receive this technique include people with high cardiac risk, severe vascular disease or allergies to the medication.
Pediatric patients are also not candidates for this kind of surgery.
What should I know if I am apprehensive about the procedure?
Patients who are apprehensive should know that this procedure is very safe and is becoming increasingly popular throughout the world. If patients are not sure about the safety of the medication, they can keep in mind that the anesthesia medication used in WALANT procedures is the same that dentists use daily.
Patients who have a WALANT surgery commonly say that it was a lot easier than they thought it would be after surgery. WALANT patients are usually very happy and recommend the technique to their friends and family. Most patients become less anxious once they see that it’s not painful, and Washington University surgical teams provide comfort and distractions for patients if they need it.
What should referring physicians know about WALANT at WashU?
Currie is currently taking patients for WALANT procedures at Christian Northeast and Alton Memorial Hospital. Both hospitals are a part of the BJC HealthCare system and affiliated with Washington University School of Medicine. Washington University Physicians is a highly active clinical practice group and is one of the largest academic clinical practices in the United States. Receiving care at an academic medical center means patients will receive care from top doctors with the latest applications of approved clinical research.
How do I contact to learn more about WALANT hand surgery?
For more information or to schedule a WALANT appointment with a Christian Hospital or Alton Memorial Hospital surgeon, call 314-362-7388 or request an appointment online.