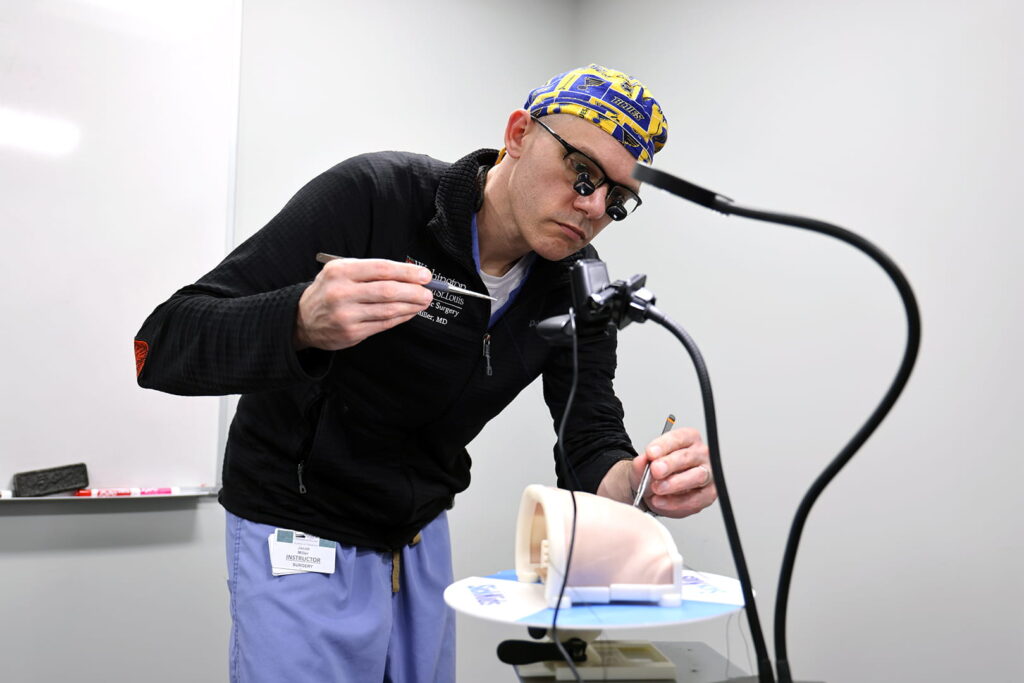
After gaining valuable experience during an in-depth, hands-on training experience, Washington University pediatric cardiothoracic surgeons and fellows can utilize new tools to diagnose and plan treatment strategies for patients with rare and complex heart defects.
Surgeons in the Division of Cardiothoracic Surgery recently joined in on a specialized training program tailored around treating congenital heart defects. The HOST (Hands-On Surgical Training) program, led by cardiovascular surgeons from the Hospital for Sick Children in Toronto, Canada, guided surgeons from around the world through the surgical repair of complex heart defects utilizing realistic simulation models. The team from Washington University were the only surgeons from the United States that participated in the session.
Though the Section of Pediatric Cardiothoracic Surgery currently utilizes 3D models in preoperative planning, trainee education and patient education at St. Louis Children’s Hospital, the HOST program gave the surgeons a new perspective in treating congenital heart conditions.
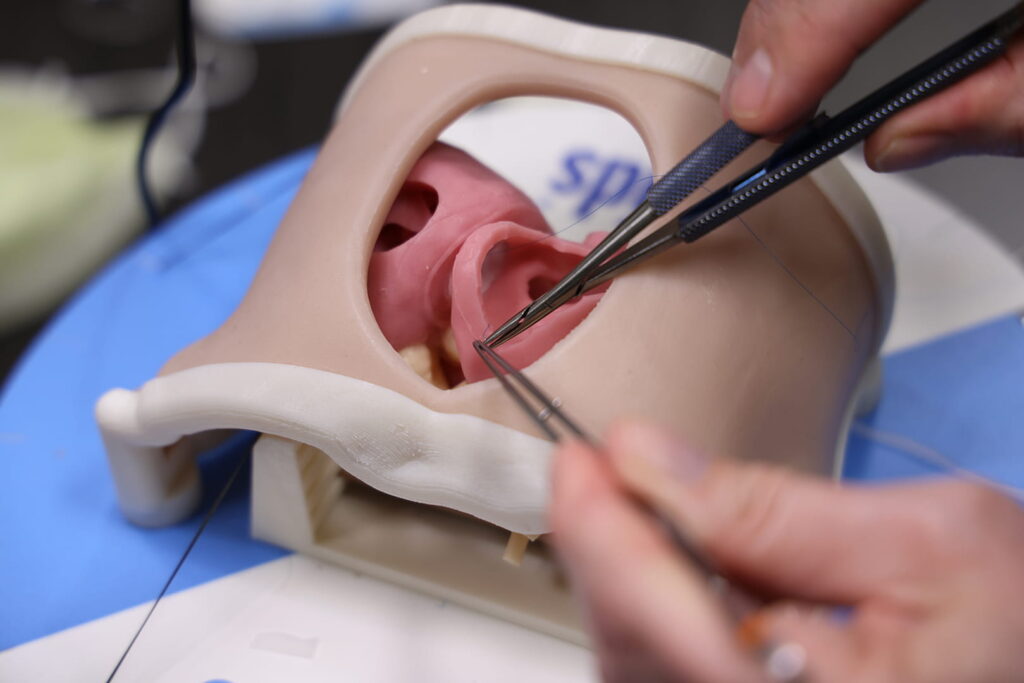
“We were astounded by the level of detail shown in the specially prepared silicone models used in this program,” says Pediatric Cardiothoracic Surgery Section Chief Pirooz Eghtesady, MD, PhD. “The models, designed in accordance with real defects captured by CT or MRI imaging, were 3D-printed, assembled and shipped to our team.”
When the models arrive at their destinations, each model is mounted to a base and stand and outfitted with a webcam and lighting equipment, allowing the program proctor to see the surgeons’ techniques in real time in the program’s virtual environment.
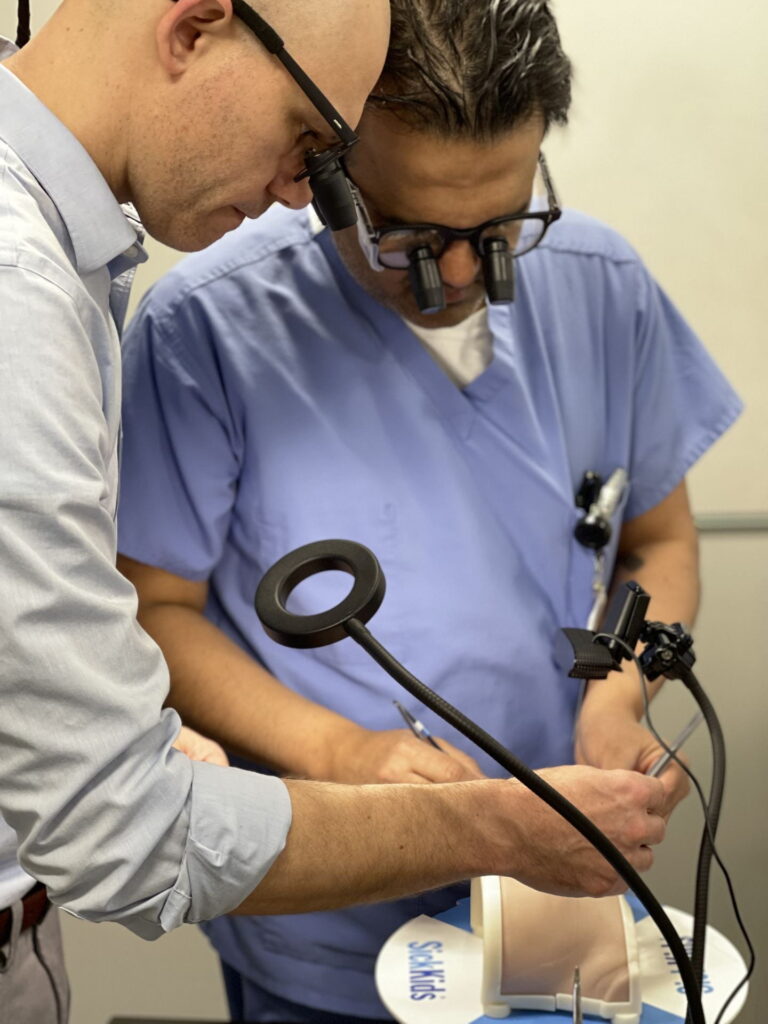
Following an introductory preparatory course prior to the HOST program’s sessions, trainees and faculty members practiced simulated procedures on the complex models with guided instructions. Thoracic surgery fellow Whitney Brandt, MD, performed an extended end-to-end coarctation aorta repair on a newborn model. Congenital cardiac surgery fellow Vinod Sebastian, MD, and instructor Jacob Miller, MD, practiced Norwood procedures. The Norwood technique is used to repair defects like hypoplastic left heart syndrome and double inlet left ventricle with malposed great vessels, interrupted aortic arch with ventricular septal defect, and coarctation with arch hypoplasia.
“The HOST program is a useful course for surgeons at all stages of their career,” says Sebastian. “The models we have used are very accurate depictions of real congenital heart disease patients and the tissue quality is strikingly similar to real neonatal tissue.”
“In patients with complex disease, these models provide a great resource and allow for one to really visualize pathology. The models the closest thing to mimic actual surgery that I’ve ever seen,” says Miller. “They also act as a great reference to facilitate discussion with the faculty and discuss tips and tricks used to optimize the repair.”
“Since the session was conducted in a virtual environment with a webcam spotlighting the surgical area and model, surgeons received real-time feedback from the course proctors during their procedures and received a final review of their approaches and anatomic results,” says Eghtesady, who is cardiothoracic surgeon-in-chief at St. Louis Children’s Hospital. “We are happy to report the patients did well under the hands of our surgeons.”
Eghtesady said the division plans to conduct a modified version of the training program monthly and suspects it will become a popular course within its comprehensive surgical training curriculum.