Washington University acute and critical care surgeons specialize in traumatic injuries, emergency surgeries, geriatric trauma, general surgeries, burn and wound care, and critical care. They provide top-quality care to a high volume of diverse cases at Barnes-Jewish Hospital, a regional referral center for critically ill patients and designated Level I Trauma Center by the State of Missouri. These surgeons collaborate with intensivists from the Washington University Department of Anesthesiology and Division of Emergency Medicine. Trainees are exposed to a large, diverse patient population and receive mentorship from nationally recognized surgical leaders while treating complicated cases on several intensive care units.
Our Year In Numbers

6,851
operating room cases

47,057
visits

37
faculty

2,267
office procedures
86
clinical research studies

$922,747
research funding
Section of Acute and Critical Care Surgery | 2022 Annual Report
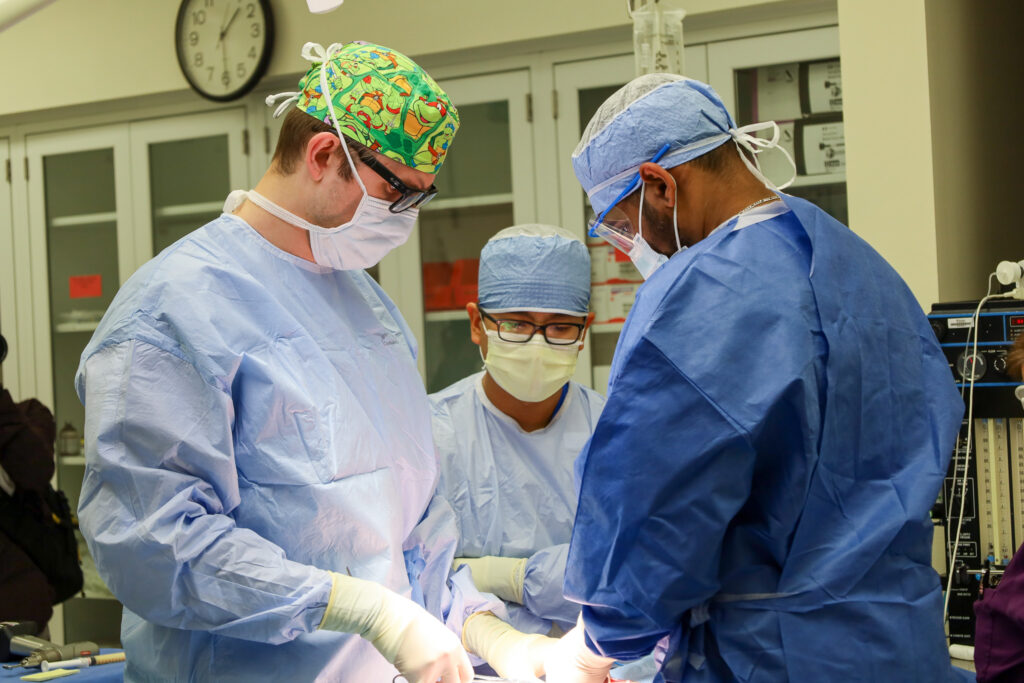
For patients with traumatic injuries or acute illness, every second counts. The Washington University surgical care surgery fellowship prepares surgeons to recognize and address the myriad needs of this patient population through immersive clinical experience and simulation training. Led by Program Director Sara Buckman, MD, PharmD, the surgical critical care fellowship offers multidisciplinary training at Barnes-Jewish Hospital, the #1 hospital in St. Louis and Missouri and #11 in the nation, according to U.S. News & World Report.

The Washington University limb preservation program consists of a multidisciplinary team of physicians who utilize cutting-edge techniques and a collaborative approach to provide emergency and ongoing care in preserving the form and function of limbs. This June, podiatrist Neil Ermitano, DPM, joined the Section of Acute and Critical Care Surgery as an assistant professor, with a clinical focus on detecting and treating limb-threatening conditions, diabetic foot and wound care, and treating trauma and infections.
Highlights
CLINICAL

The Washington University limb preservation program consists of a multidisciplinary team of physicians who utilize cutting-edge techniques and a collaborative approach to provide emergency and ongoing care in preserving the form and function of limbs. This June, podiatrist Neil Ermitano, DPM, joined the Section of Acute and Critical Care Surgery as an assistant professor, with a clinical focus on detecting and treating limb-threatening conditions, diabetic foot and wound care, and treating trauma and infections. “This section is special in that it provides a very team-based approach to patient care and treatment,” Ermitano says. “I look forward to contributing to its already vast fund of knowledge and expertise to help serve the St. Louis area.”
RESEARCH

Faculty in the Section of Acute and Critical Care Surgery lead multiple Department of Defense-funded research projects, including a recent clinical trial of the drug tranexamic acid (TXA), which is routinely given to critically injured patients experiencing severe blood loss. The TAMPITI trial, led by Grant Bochicchio, MD, chief of acute and critical care surgery, suggests the drug may have only minimal effects on blood clotting when use to treat a recent, massive injury. A subsequent study published in the journal Transfusion found a dose-dependent increase in the risk of thromboembolism due to TXA in patients with severe traumatic injury, underscoring the need for thromboembolism screening in appropriate patients receiving TXA.
EDUCATION

The Section of Acute and Critical Care Surgery plays an integral role in surgical education at the School of Medicine. General surgery residents rotate through the critical care service, gaining valuable experience treating traumatic injuries and critically ill patients. Residents are also trained in simple to complex minimally invasive surgery in the OR, including procedures like video assisted thoroscopic surgery. While rotating on the critical care service, current resident Katharine Caldwell, MD, said of the residency: “We have an incredible program. I couldn’t have been happier to spend the last seven years here.”

Unparalleled Experience
For patients with traumatic injuries or acute illness, every second counts. The Washington University surgical care surgery fellowship prepares surgeons to recognize and address the myriad needs of this patient population through immersive clinical experience and simulation training.
Led by Program Director Sara Buckman, MD, PharmD, the surgical critical care fellowship offers multidisciplinary training at Barnes-Jewish Hospital, the #1 hospital in St. Louis and Missouri and #11 in the nation, according to U.S. News & World Report. The trauma center at Barnes-Jewish Hospital was the first in Missouri to receive Level I verification from the American College of Surgeons (ACS) and remains the busiest trauma center in the state.
Fellows train in the multidisciplinary surgical/burn/trauma and cardiothoracic intensive care units with elective opportunities in numerous other disciplines tailored to meet the fellow’s goals. Early in his fellowship, Karthik Sugurmaran, MD trained in critical care, trauma, cardiac intensive care and critical care ultrasound.
Washington University are truly unmatched,” says Buckman. “During your fellowship, you will work closely with experts in the field of critical care, distinguished research investigators and leaders who are defining the future of surgical critical care on a national and international level.”
Outside the clinical setting, fellows gain valuable experience through simulation training at the Washington University Institute for Surgical Education (WISE), an ACS Level 1 Accredited Education Institute. WISE offers a variety of trainings and certifications, including robotic and laparoscopic labs, for learners ranging from residents and fellows to allied health professionals and practicing physicians.
“In the simulated environment, a fellow can practice trauma exposure maneuvers and become familiar with aspects of a procedure with no impact on patient care,” says Thoi Ngo, MD, an assistant professor of surgery. “We can prepare fellows in a non-emergent setting. Then, when an acute patient presents, the fellow is ready to respond quickly and capably.”
In addition to sharpening their surgical skills, fellows gain valuable experience as educators. Sugurmaron recently led a training session for attending pediatric physicians. “The opportunity to step into the role of the educator prepares you for a career in academic medicine. It also allows you to apply what you’ve learned during your own training,” Sugurmaran says. “The fellowship truly offers an unparalleled experience in critical care.”

Life Outside of Violence
The impacts of violence-related trauma go beyond the emergency room–the physical injuries are only one part of the cycles of perpetuated violence within communities. Some estimates report nearly 60% of people who experience violence-related trauma in the U.S. will later return to the hospital for similar reasons.
Launched in 2018 by Washington University’s Institute for Public Health, the Life Outside of Violence (LOV) program is promoting an individualized approach to disrupting cycles of violence and working to support victims of violent trauma. LOV offers comprehensive support to those who have experienced violence with the goal to reduce retaliation, re-injury and death. LOV offers services to provide participants with mental health services, resources for education and employment, and medical and housing assistance.
Trauma surgeon Douglas J. E. Schuerer, MD, is the director of trauma at Barnes-Jewish Hospital and a founding board member of the LOV program. “It has been very important to us as providers because we’re finally starting to affect injury prevention in and around the area of interpersonal violence,” says Schuerer. “That’s been one of the hardest areas to address.”
Participants in the LOV program are connected to a case manager who functions as a point of contact for comprehensive support. LOV provides participants with resources that bolster their journey toward recovery, which heals both individual and community alike. “It’s important for us to demonstrate the benefits of the program to the community, to foster more trust toward the medical system,” Schuerer says.
LOV is the first city-wide, hospital-based violence intervention program in the United States, and it is collaborative between institutions. Four trauma centers, including Barnes-Jewish Hospital and St. Louis Children’s Hospital, collaborate with three research universities: Washington University, Saint Louis University and University of Missouri-St. Louis. The collaborative effort has broadened the program’s reach and has allowed it to get a better perspective on how violence and its impacts on the city.
“By collaborating among hospitals citywide, we have a more robust program, and we’re able to track and understand the patients and outcomes a lot better than any single institution,” says Schuerer. Program data includes the number of people citywide subjected to violence and the amount of recidivism after the first encounter with violence, information which is valuable to decreasing these cycles.
Over four years, LOV has already seen dramatically lower rates of recidivism for patients who have enrolled in the program’s support system, achieving its goal of less than 10% recidivism within its first three years of operation. Even more impressive, there have been no incidents of retaliation or mortality among the enrolled participants. These results are further telling of LOV’s effectiveness at providing mental health care and breaking cycles of violence.