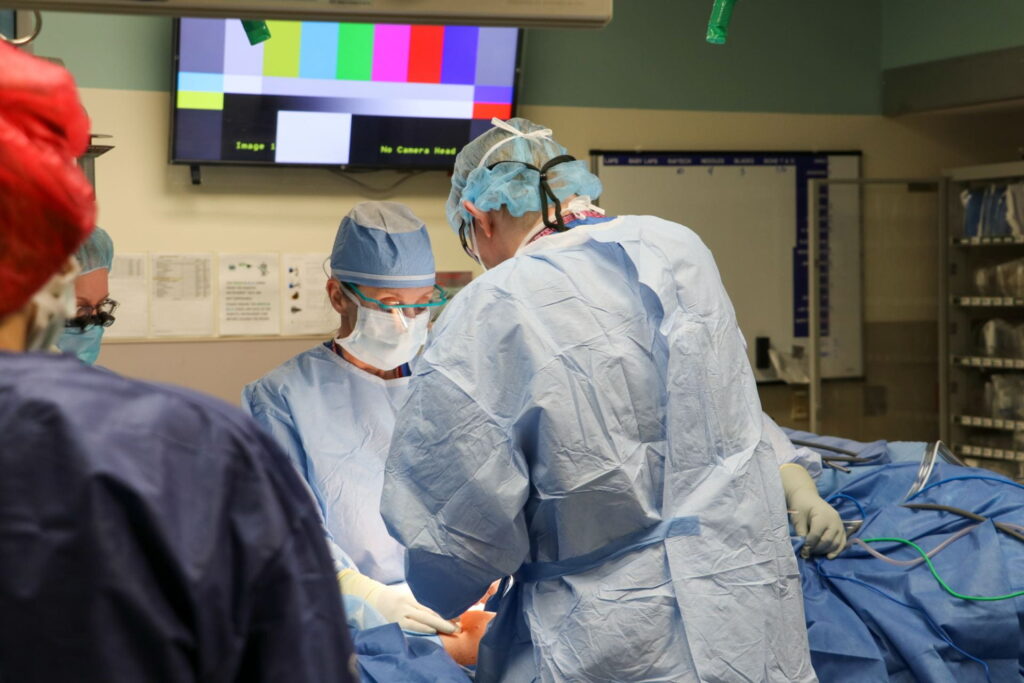
This section has a long, successful history and offers the latest advancements in the field. In liver transplantation, the program offers living-related and living-unrelated donor, reduced-size liver, split liver and dual-organ transplantation. Faculty offer both laparoscopic and “mininephrectomy” kidney donor procedures. Transplant surgeons are leaders in islet cell transplantation and have the largest pancreas transplant program in the region. Along with their clinical expertise, faculty are leaders in the field of transplantation research and train fellows in a nationally recognized, two-year certified program.
1,210
Operating room cases
11,310
Visits
8
Faculty
65
Clinical research studies
$1,063,197
Research funding
Section of Transplant Surgery | 2021 Annual Report

Transplant surgery fellowship programs provide trainees exposure to advanced techniques in the surgical and medical management of patients with end-stage organ disease. Washington University Abdominal Organ Transplant fellows develop proficiency in transplantation by participating in a volume of cases far exceeding requirements set by the Transplant Accreditation & Certification Council.

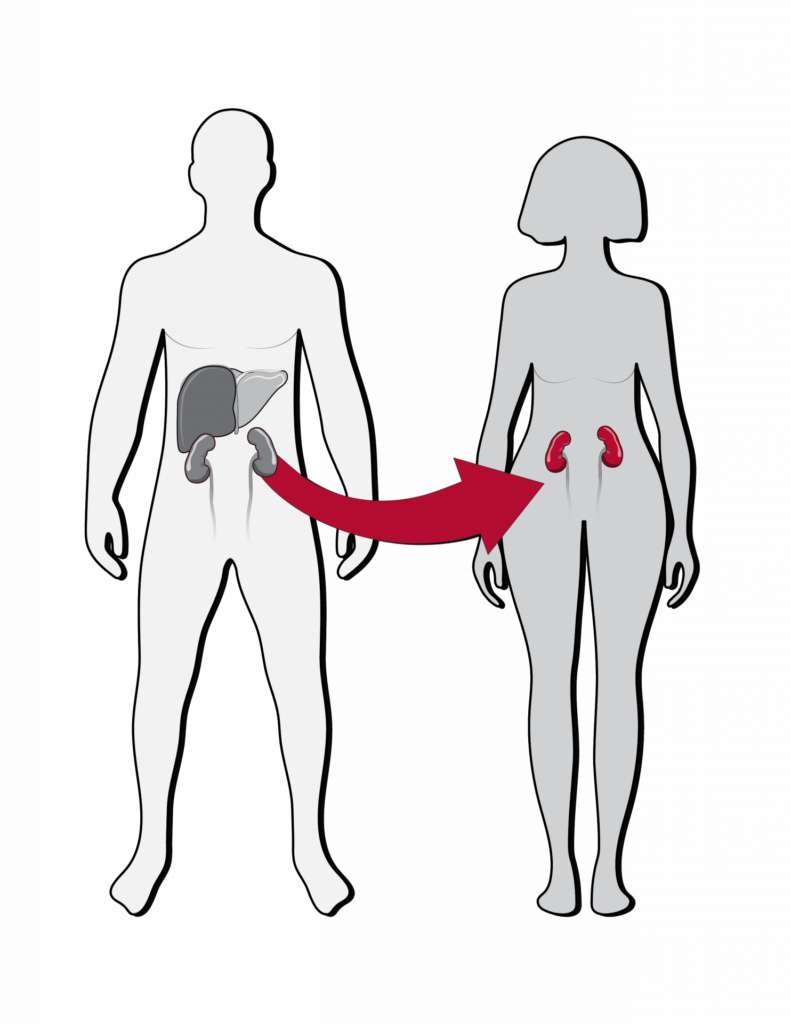
There are approximately 100,000 people in the United States waiting for a life-saving kidney transplant, according to the Organ Procurement and Transplantation Network. While most donor organs come from deceased donors, the wait time for a deceased donor kidney can be three to four years or more.
Section of Transplant Surgery Highlights | 2021 Annual Report

Clinical
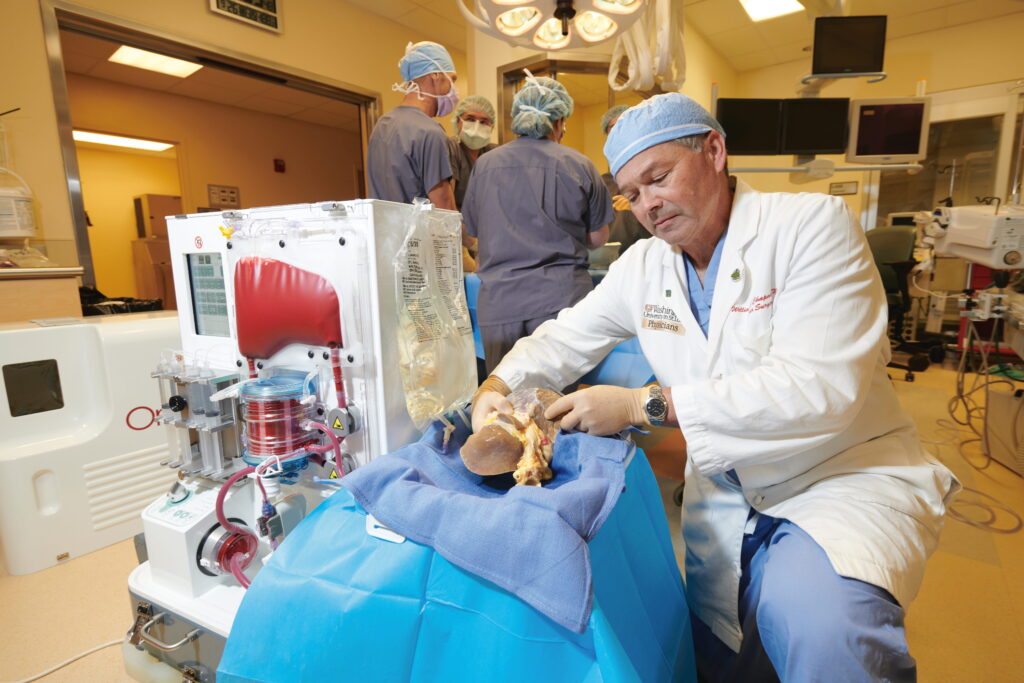
The need for liver transplants far exceeds the number of available organs. Transplant Section Chief William Chapman, MD, is principal investigator on a clinical trial using normothermic machine perfusion (NMP), a method of organ preservation that could make marginal or unsuitable livers viable options for transplant. Seventy percent of livers treated with NMP in Phase I of the trial were then suitable for transplantation and have shown good initial function. The clinical trial now enters Phase II, where more organs will undergo NMP. If successful, the trial may increase the number of transplantable livers.
Research
Liver transplant is considered the treatment of choice for nonresectable early-stage hepatocellular carcinoma. Recurrence for hepatocellular cancer following liver transplant is uncommon. For about 10-20% of patients, however, this form of cancer can recur after transplant. Washington University transplant surgeons and researchers are investigating ways of predicting and reducing a patient’s risk of recurrence. Transplant Section Chief William Chapman, MD, is local Principal Investigator of a multicenter study using cell-free DNA as a marker to determine if there is still active tumor following treatment, which could help physicians develop treatment plans to target recurrent hepatocellular cancer.

Education
The American Society of Transplant Surgeons (ASTS) requires a minimum of 45 liver transplant cases during fellowship to receive certification. In a recent study, Washington University transplant surgeon Adeel Khan, MD, MPH, assessed the liver transplant fellowship learning curve, examining measures of efficiency and outcomes, such as operative time and biliary complications. The study, published in the American Journal of Transplantation, validates the ASTS minimum, but shows consistent, sustained improvement after 45 cases. Washington University transplant fellows regularly participate in a number of cases far exceeding ASTS requirements. In 2020, the section performed 140 liver transplants.

Training the Best and Brightest
Transplant surgery fellowship programs provide trainees exposure to advanced techniques in the surgical and medical management of patients with end-stage organ disease. Washington University Abdominal Organ Transplant fellows develop proficiency in transplantation by participating in a volume of cases far exceeding requirements set by the Transplant Accreditation & Certification Council. Fellows at the School of Medicine also develop valuable basic and clinical research, leadership and mentorship skills during their training.
Senior fellow Jennifer Yu, MD, MPHS, received the 2020-2021 Gregorio A. Sicard Fellow Teaching Award for her performance in educating and training general surgery residents. Training residents, medical students and sub-interns during fellowship prepares fellows for careers in transplant surgery at academic medical centers.
“Jennifer has a reputation of going the extra mile to help everybody on the team,” says Transplant Section Chief and Eugene M. Bricker Chair of Surgery William Chapman, MD. “And that includes the patient, the nursing staff, other trainees, her peers and especially those who are coming up in their training. She is an excellent surgeon with an endearing personality and the ability to mentor her fellow trainees.”
First year transplant fellow Darren Cullinan, MD, MSCI, received the 2020-2021 Keith D. Amos Memorial Award, commemorating its namesake’s dedication to leadership, education, and patient service and outreach. Cullinan joins the fellowship after graduating from the Washington University General Surgery Residency as a Walter F. Ballinger II Administrative Chief Resident. During residency, Cullinan developed a pancreatic cancer clinical trial with the mentorship of Washington University HPB surgeons.
Greg Martens, MD, PhD, joins the program as a first-year fellow after completing his general surgery residency at the University of Alabama, where he served as administrative chief resident during his final year of training. Martens, who has a background in education and translational research, earned his PhD with a focus in xenotransplantation, which truly represents the next frontier in transplant surgery.
Fellowship Program Director Maria B. Majella Doyle, MD, MBA, fosters leadership skills in fellows as well as faculty in the Department of Surgery through her involvement in the Faculty Development and Mentoring Program. As Chair of the Vanguard Committee of the American Society of Transplant Surgeons, Doyle further advances the engagement of transplant surgeons in leadership initiatives at a national level.
“By creating a better work-life balance and more diverse leadership, we are attracting the best and the brightest trainees to become surgeons,” says Doyle. “We have challenges ahead, from achieving health equity to building trust between patients and physicians, but I also believe we have a bright future as long as we remain engaged in all facets of academic surgery.”

Living Donor Champions
There are approximately 100,000 people in the United States waiting for a life-saving kidney transplant, according to the Organ Procurement and Transplantation Network. While most donor organs come from deceased donors, the wait time for a deceased donor kidney can be three to four years or more. Many waitlisted patients with kidney disease become too sick for transplantation before being matched with an available organ.
Washington University transplant surgeons have increased their focus on living organ donation to address this growing need. As Surgical Director of Kidney and Pancreatic Transplantation at the Washington University and Barnes-Jewish Transplant Center, Jason Wellen, MD, MBA, is leading the Live Donor Champion Program at the School of Medicine.
Many kidney transplant candidates feel uncomfortable or ill-equipped to ask others to consider donating. A Live Donor Champion is a spouse, significant other, family member or friend who serves as an advocate for the candidate.
“It’s a hard topic to broach,” says Wellen. “If you feel uncomfortable asking people to consider organ donation, find a friend or a loved one who will fight that battle for you. Let them be your champion.”
The Live Donor Champion Program provides Champions with education and advocacy training to help them seek out potential donors. In pilot studies, participants with a Live Donor Champion were more likely to undergo live donor kidney transplant than other transplant candidates. The kidney transplant team continues to refine the Live Donor Champion Program to best fit the needs of patients. Patients involved in the program have emphasized the value of having a donor champion and encourage future patients to participate in the program.
Living donors can significantly accelerate the transplant process. A compatible living donor organ can be transplanted within months, rather than waiting years for a deceased donor match. The transplant program also participates in paired-donor kidney exchanges, frequently finding matches for multiple transplant candidates across the country.
The Transplant Surgery Section, which performed over 300 kidney transplants in 2020, has also taken steps to improve the organ donation experience. Washington University transplant surgeons perform robotic donor nephrectomy. The minimally invasive technique offers improved 3D visualization, fine motor control and wristed motion for the surgeon, while typically reducing pain, length of stay and recovery time for donors.
“Our goal is to get every eligible candidate transplanted,” says Wellen. “It’s very touching to see how many lives we are able to change.”