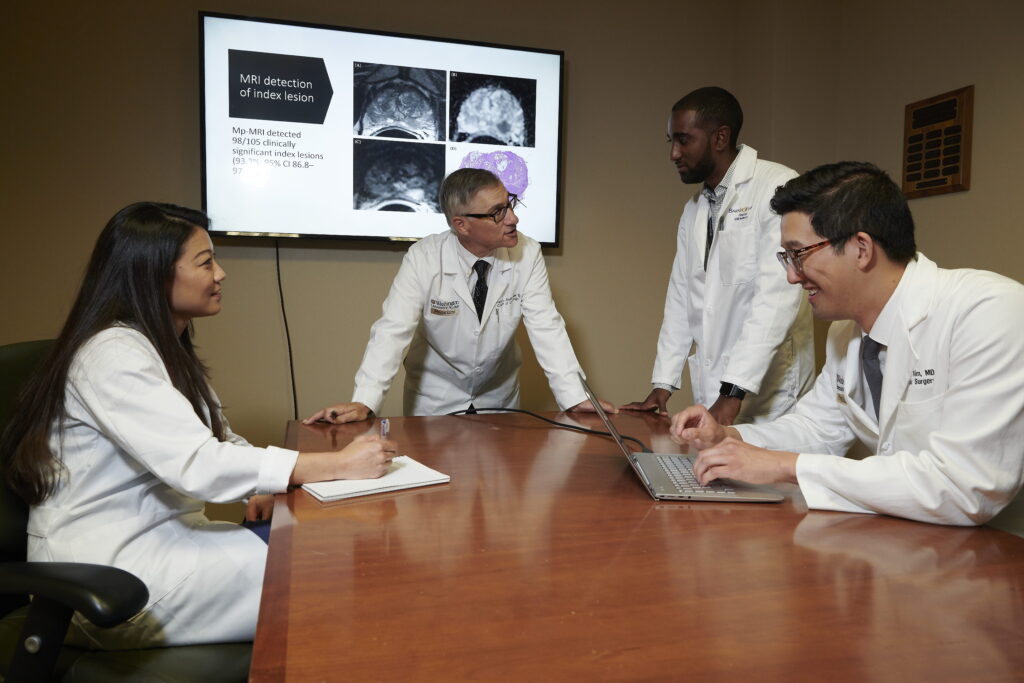
Faculty in this division are leaders in the field of urology and minimally invasive surgical techniques. Urologists offer a range of treatment options, both surgical and nonsurgical, for medical conditions of the urogenital tract, including the prostate and testicles in males and the kidneys and bladder in both males and females. The division is also nationally recognized for its research on detecting and determining the level of risk of prostate cancer. The urology residency and fellowship programs train outstanding physicians through the expertise of fellowship-trained faculty, high volume, diversity of cases and spirit of inquiry.
7,793
Operating room cases
48,632
Visits
26
Faculty
12,455
Office procedures
70
Clinical research studies
$4,879,404
Research funding
Division of Public Health Sciences | 2021 Annual Report
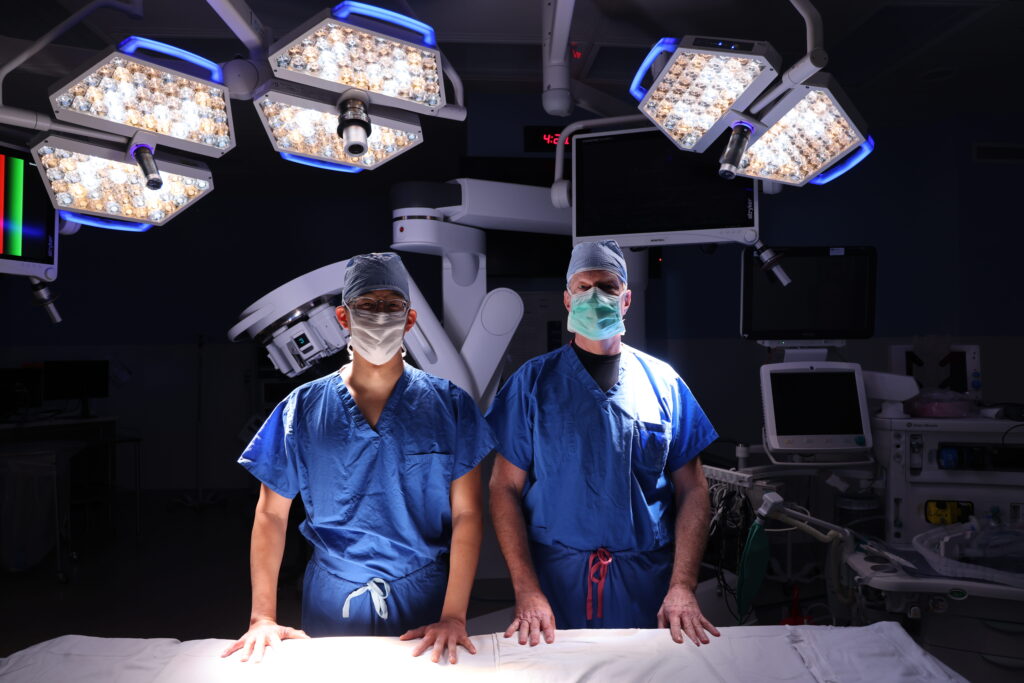
Washington University urologists are leading clinical investigations targeted towards developing more personalized cancer care. Clinical studies in the division continue to advance methods of diagnosing and treating urologic cancers.

In 1921, the Washington University Urology Residency Program accepted its first intern. The program celebrates its centennial by recognizing historical contributions to field of urology and continuing this tradition of excellence in urologic training.
Division of Urologic Surgery Highlights | 2021 Annual Report
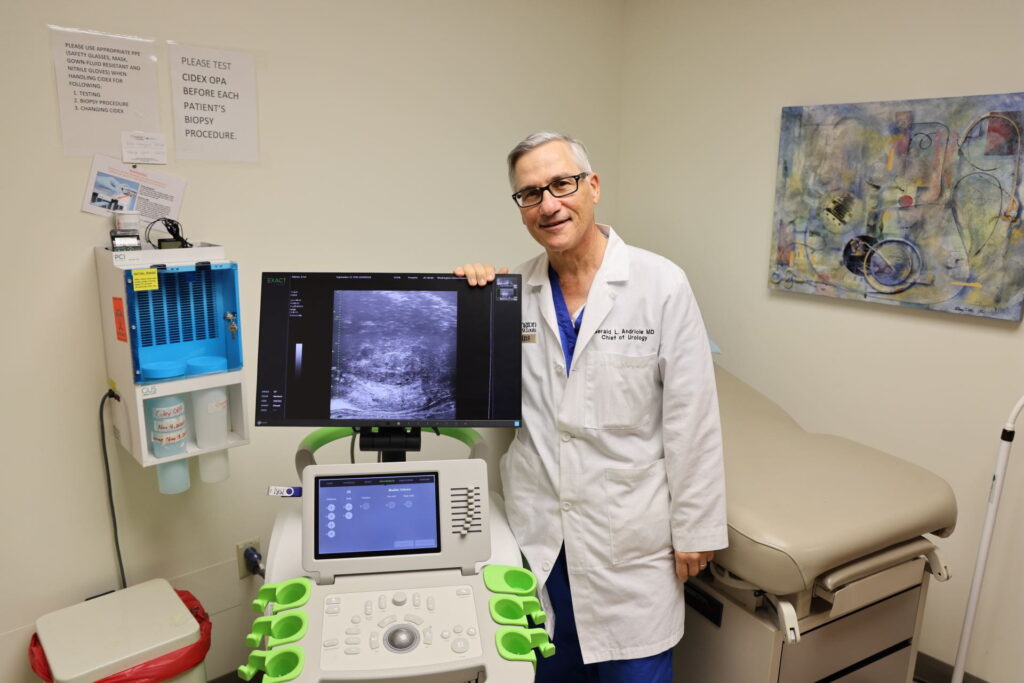
Clinical
In a multi-year effort, the Division of Urologic Surgery and BJC HealthCare have united to provide world-class Washington University urologic care at nine clinical locations across the St. Louis area and Illinois. This ongoing partnership aims to enhance quality of care, increase access to health services and reduce the total cost of care across the hospital system. “By providing the same high level of urologic care at each location, we can standardize care for patients on both sides of the river,” says Division Chief Gerald Andriole, MD, the Robert K. Royce Distinguished Professor of Urologic Surgery, who led the initiative.

Research
Washington University urologist Alana Desai, MD, is leading a study to examine stent-associated pain in urinary stone disease patients after ureteroscopy. “Stone disease can be painful enough,” Desai says. “If we can identify those at risk for severe stent pain, we can better address their pain through future studies.” Desai and Professor of Surgery Henry Lai, MD, are co-principal investigators on multiple projects investigating urinary stone disease prevention, symptoms and treatment, funded by the National Institute of Diabetes and Digestive and Kidney Diseases and the Urinary Stone Disease Research Network.

Education
The Division of Urology now offers a Society of Urologic Oncology (SUO) Fellowship led by Program Director Zachary Smith, MD. The SUO-accredited fellowship provides in-depth experience in open, laparoscopic, robotic and reoperative surgery for all urologic cancers. Fellows collaborate with radiation oncologists and medical oncologists for comprehensive training in every aspect of urologic malignancy. The two-year program, which accepts one fellow per year, comprises one year of clinical and one year of research experience. Cayce Nawaf, MD, the inaugural fellow, completed urology residency training at Yale School of Medicine.
Personalizing Urologic Cancer Care
Washington University urologists are leading clinical investigations targeted towards developing more personalized cancer care. Clinical studies in the division continue to advance methods of diagnosing and treating urologic cancers.
Eric Kim, MD, is principal investigator of a study evaluating the use of Diffusion Basis Spectrum Imaging (DBSI) for early detection of prostate cancer. DBSI is a novel MRI parameter that may help urologists detect prostate cancer sooner and determine appropriate treatment.
Focal ablation allows physicians to target only the cancerous portion of the prostate for patients with localized cancer. Washington University urologists, including Kim, are participating in a multi-center study to determine the efficacy of using MRI/ultrasound fusion imaging technology to direct focal ablation of prostate tissue using nanoparticle-directed laser ablation.
Zachary Smith, MD, and a multidisciplinary team of researchers are investigating the ability of checkpoint inhibitor immunotherapy to improve the condition of patients with initially unresectable kidney cancer. After receiving this immunotherapy, some patients were able to undergo cytoreductive nephrectomy. Future studies aim to predict which patients will respond to immunotherapy and become surgical candidates.
“We are trying to understand who will respond to which therapy,” says Smith. “When we can predict how you will respond to immunotherapy or chemotherapy, we can develop truly personalized medicine for patients with urologic cancers.”
Smith, radiation oncologist Aadel Chaudhuri, MD, PhD, and medical oncologist Vivek Arora, MD, PhD, are developing a urine test to study the DNA of muscle-invasive bladder cancer patients treated with radical cystectomy.
“For bladder cancer, if a urine biopsy can detect whether the early chemotherapy totally eradicated the tumor, it could help some patients avoid major surgery to remove the bladder,” says Chaudhuri.
While there are existing urine tests that can help identify bladder cancer, these can be imprecise. Cystoscopy is more precise, but also more invasive. A DNA-based urine test could prove to be more sensitive by identifying any residual disease following cystectomy, and more specific than other urine tests, which can provide false-positive results.
“Personalized cancer care means that we will be able to tailor our treatment plan to each individual,” says Division Chief Gerald Andriole, MD, the Robert K. Royce Distinguished Professor of Urologic Surgery. “We have excellent treatment options, and these advances will help us know in advance which will work best for each patient.”

100 Years of Urology Training
In 1921, the Washington University Urology Residency Program accepted its first intern. The program celebrates its centennial by recognizing historical contributions to field of urology and continuing this tradition of excellence in urologic training.
Over the past century, Washington University School of Medicine has become a national leader in urologic surgery. Faculty have continuously made major contributions to patient care, from pioneering transurethral prostatic resection to introducing techniques for ileal conduit urinary diversion and developing PSA testing for prostate cancer. Washington University urologists were also early leaders in laparoscopic surgery, performing the first laparoscopic nephrectomy in 1990. Faculty today continue to advance new approaches to all forms of urologic cancers, minimally invasive surgery, reconstructive urology, stone disease, men’s health problems and other conditions.
“Washington University Urology has been on the cutting-edge since urology became a field,” says Urology Residency Program Director Erica Traxel, MD. “I am proud to be part of a division and program with such a rich history.”
In its hundredth year, the residency program builds on this rich history by training residents in the latest techniques and technologies. At the Washington University Institute for Surgical Education (WISE), trainees practice complex procedures, such as partial nephrectomy and robotic prostatectomy. Expert faculty lead skills labs in endourology and other areas of urologic specialization, introducing residents to the newest innovations in technique.
“The landscape of residency training has changed significantly over the past hundred years,” says Assistant Program Director Jason Frankel, MD. “We are developing educational programming and pedagogy. We are becoming more intentional about the way we train the next generation of urologists.”
Assistant Professor of Surgery Kefu Du, MD, has formalized robotics curriculum in the division. Faculty offer conferences dedicated to patient safety and quality improvement. Residents receive training to understand and address inequities in access to medical care.
Traxel and Frankel aim to bring a new level of academic structure to urologic training. Frankel is completing a graduate degree in education. In 2020, Traxel was inducted to the Academy of Educators at the School of Medicine. Traxel has also been a member of the Office of Medical School Education Gateway Curriculum Immersion development team.
“It takes more than training someone to understand a disease process or steps of an operation,” says Traxel. “We are training residents to see patients as human beings. We are training residents to maintain their own wellness. Washington University is expanding the scope of urologic education and training.”